Image Credit: ThamKC/shutterstock.com
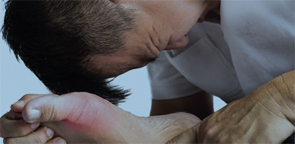
Gout affects nearly 4% of American adults, causing joint inflammation, pain and crystal deposits that may lead to bone erosion over time. At least five different classification criteria for gout are used worldwide, creating potential discrepancies in clinical trial enrollment and eventual results.
An international panel of investigators collaborated to create new, standardized gout classification criteria by conducting a multi-phase study of hundreds of gout patient cases. The panel members hope the new criteria will enable any rheumatology clinical researcher—no matter where a study or trial is conducted—to identify and enroll a more homogenous set of gout patients. In turn, this may facilitate more effective gout studies, including clinical trials for new treatment development. The criteria were released by the American College of Rheumatology (ACR) in conjunction with the European League Against Rheumatism (EULAR) and simultaneously published in Arthritis & Rheumatology and Annals of the Rheumatic Diseases in October 2015.
“We wanted to determine what features of gout best distinguish it from other conditions that could be similar to gout,” says Tuhina Neogi, MD, PhD, associate professor of medicine in the Boston University School of Medicine and one of the lead investigators in the study. “The new classification criteria incorporate patients’ symptoms, physical exam findings, serum uric acid levels, joint fluid analysis, X-ray findings and advanced imaging findings.”
The new ACR/EULAR gout classification criteria are a significant improvement over previous versions, says Tim L. Jansen, MD, PhD, one of the investigators and a rheumatologist at VieCuri Medical Center in Venlo, The Netherlands.
“The new criteria are to be used in anyone with suspected gout. And they have a very good sensitivity and specificity, much better than older criteria,” he says. “We needed newer criteria [because] ultrasound as a tool was not included in previous ones. We also knew that older criteria lacked validation, and 20% of patients could not be classified. Specificity was low in old criteria sets due to the inclusion only of advanced gout cases,” whereas the new criteria also include newer cases.
The new criteria have numerous possible benefits for researchers, says Dr. Jansen.
“New drugs can be tested in a better-defined group of patients and that will help significantly. Also, epidemiologic data, reflecting mortality on a U or J curve, or new tests, for example, new cell-based gout tests, can be studied better,” he says.
The investigators identified entry, sufficient and exclusion criteria for patient cases to include in the study. The entry criteria were intended to be used to identify the relevant patient population to whom the classification criteria would be applied. Sufficient criteria were intended to define a gold standard, features that alone could classify gout without further need to apply the classification criteria scoring system. Exclusion criteria were intended to define individuals in whom gout could be ruled out (among those who met entry criteria) and to whom the classification criteria should not be further applied.