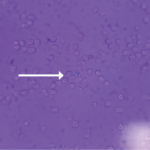
Exciting molecular genetic advances in CPPD have been spurred by identification of linkage of familial, early-onset CPPD with multiple mutations in ANKH.7,8 Moreover, homozygosity for -4 G to A substitution in the ANKH 5’-untranslated region, which promotes increased ANKH mRNA levels, was present in approximately 4% of British subjects who had carried a prior diagnosis of idiopathic chondrocalcinosis of aging.13 Increased ANKH promotes cartilage matrix catabolism by chondrocytes.8 As such, ANKH mediates development and anatomic progression of both early-onset familial CPPD and late-onset disease.
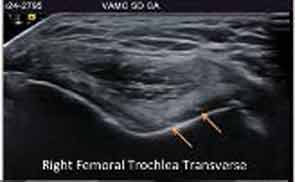
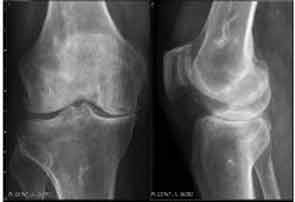
New Developments in CPPD Clinical Features and Outcomes
A recent consensus process by the European League Against Rheumatism (EULAR) reclassified CPPD, and suggested new terminology for clinical forms of CPPD arthritis.14 EULAR’s proposed abandonment of the “pseudogout” terminology for acute CPPD arthritis ultimately may be counterproductive for disease recognition outside rheumatology. Other limits of the EULAR classification, in my opinion, include lack of precise attention to systemic degenerative arthropathy primarily driven by CPPD in a subset of patients, rather than secondarily associated with the primary process of OA in the majority. In this context, chronic degenerative arthropathy in primary CPPD commonly affects certain joints that are typically spared by primary OA, such as the metacarpophalangeal and wrist joints.15
CPPD is very often clinically silent, but is a biomarker of aging, connective-tissue degeneration, and low-grade inflammation.15 Because CPPD is so strongly linked with OA, and can manifest as a primary cause of inflammation and cartilage-matrix catabolism, the impression has been that CPPD drives inflammatory symptoms and progression in OA. However, there is no clear correlation between the extent of calcification and progression of CPPD. The Boston Osteoarthritis of the Knee Study and the Health, Aging, and Body Composition Study did not link CPPD with elevated risk of cartilage loss in OA.16 Other work revealed no significant differences with or without CPPD in activities of daily living, or age at total knee arthroplasty, for degenerative arthritis.15 Moreover, the association between OA and CPPD may be linked more to presence of osteophytes than to joint-space narrowing.15