Dr P. Marazzi / Science Source
A recent study explored medical concerns for patients who have lupus markers, but fall short of meeting enough criteria for official disease classification.
Investigators at the Oklahoma Medical Research Foundation conducted a large study to explore current treatments of patients with incomplete lupus erythematous (ILE) and to compare antibody characteristics to healthy people and patients with classified lupus. The study results appeared in the December issue of the journal Arthritis Care and Research.1
The nature of ILE remains poorly understood, and no definition or treatment recommendations for it exist, says Judith James, MD, PhD, vice president of clinical affairs at the Oklahoma Medical Research Foundation in Oklahoma City. Patients with ILE have clinical features of lupus, but don’t meet four or more criteria required under the ACR classification for systemic lupus erythematous (SLE), says Dr. James.
“For this study, we used the term ‘incomplete lupus erythematosus’ to mean the patient met three ACR classification criteria for lupus. However, ILE has also been defined as having a positive blood test plus at least one or two clinical features of lupus,” she says.
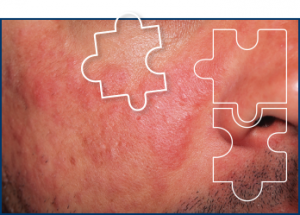
ILE patients are usually referred to a rheumatologist initially because a doctor suspected lupus or other autoimmune disease and a blood screen showed positive for antinuclear antibodies (ANAs), says Dr. James. These patients may also present such symptoms as rash, mouth sores, photosensitivity, joint pain and swelling.
In this nationwide study, researchers recruited participants through the Lupus Family Registry and Repository and examined medical records for common symptoms and medications. They used the SLE portion of the Connective Tissue Disease Screening Questionnaire to gather demographic, clinical and self-reported symptoms from participants, and measured autoantibodies to examine immunologic features.

Dr. James
Most study participants were women, and the ILE group tended to be slightly older than those in the SLE group. There were more white participants than other races, followed in number by African American and Hispanic.
In a group of 440 ILE patients given the questionnaire, the respondents reported the same number of SLE symptoms whether they were patients with major clinical manifestations of the disease or patients with minor manifestations. These symptoms included pleurisy and protein in the urine, as well as seizure.
The same questionnaire was given to 3,397 patients with SLE, who reported slightly more symptoms than patients with ILE (6.4 vs. 5.9). Both groups reported more SLE-related symptoms than people in a control group.