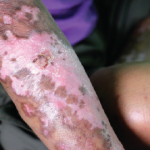
Systemic sclerosis (SSc; scleroderma) is a disease in which inflammatory and fibrotic changes result in overproduction and accumulation of collagen and other extracellular matrix proteins, resulting in intimal vascular damage, fibrosis, and occasionally organ dysfunction affecting the gastrointestinal, lung, heart, and renal systems. There are two classifications of SSc—limited cutaneous or CREST (calcinosis, Raynaud’s, esophageal dysmotility, sclerodactyly, and telangectasias) syndrome, where skin thickening occurs mainly in the distal extremities and facial/neck areas and internal organ involvement, if present, occurs later in the disease process; and diffuse cutaneous disease where there is a more rapid progression of skin thickening from distal to proximal and organ involvement can be severe and occur early in the disease.1,2 As noted by various authors, there is no “crystal ball” into which one can look to see the outcome of the disease, and involvement varies significantly from one person to the next.
The role of the nurse practitioner/physician assistant is integral in assessing the various components of disability and pain experienced by the scleroderma patient. We work closely with various disciplines, including occupational and physical therapists, who can add greatly to the everyday functioning of our patients who need braces, splints, adaptive equipment, and rehabilitation therapy to pursue cherished activities when claw deformities, skin tethering, and breathing difficulties or other organ involvement interferes with activities of daily living. Pain takes many forms with our scleroderma patients. Arthralgias and muscle tenderness, difficulty with swallowing, constipation resulting in “rabbit pellet” stools, and air hunger or subjective feelings of shortness of breath can lead to depression and disability. Medications can ease symptoms and promote quality of life, and a complete review of systems, including functional assessment, should be an integral part of every clinic visit, with therapies geared toward promoting optimal health and decreasing disability.
How exactly do we assess disability in this complex and variably presenting disease? As Sultan et al have lamented, no one to date has adequately defined the concept of disability in scleroderma, particularly across cultural lines.3 Is it the functional component or the disability component that should lend weight to our formal assessments? Several measurement tools have been identified for use in clinical trials. The Hand Mobility in Scleroderma Test (HAMIS), the United Kingdom Scleroderma Functional Score, and the Rodnan skin scoring system have been used extensively.3,4 Ultrasound is an emerging imaging technique that is readily available and noninvasive, allowing for the evaluation of dermal thickening and echogenicity.5 One tool that is validated and used extensively in the rheumatoid and osteoarthritis populations is the Health Assessment Questionnaire Disease Index (HAQ-DI), a measurement of disability evaluating eight domains of activity. A hybrid of the HAQ-DI, the Scleroderma Health Assessment Questionnaire (SHAQ), first used by Steen and Medsger, adds five scleroderma-specific visual analog scales to evaluate how Raynaud’s phenomenon, digital ulcerations, breathing, and intestinal problems as well as disease activity impact the individual patient.6 This tool has been evaluated for different construct validities, is fairly easy to use in the office as well as in clinical trials, and can be used to evaluate overall patient functioning, thus streamlining the patient visit.6