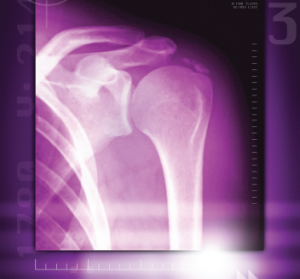
A colored X-ray of a calcified shoulder joint reveals a deposit of calcium at the top right of the shoulder joint.
Miriam Maslo / Science Source
MADRID—Calcification in osteoarthritis (OA) involves a series of pathways and interactions that feed off each other in a process that bears some resemblance to the transformation of cartilage to bone that takes place in the embryonic stage of human development, a researcher said here at the 2017 Annual European Congress on Rheumatology (EULAR).
“My hypothesis is that osteoarthritis is a restart of endochondral ossification in the adult organism,” said Jessica Bertrand, PhD, professor of orthopedic surgery at Otto-von Guericke University in Madgeburg, Germany. “The chondrocytes seem to differentiate into a more hypertrophic state, similar to endochondral bone formation.”
Dr. Bertrand’s research found this differentiation process is activated as the amount of calcification increases in vivo and in vitro. “This [finding] indicates a link between chondrocyte hypertrophy and cartilage calcification,” she said.
She described a key role of the pyrophosphate pathway, which is involved in the production of basic calcium phosphate (BCP) crystals.
In their OA cohort and in mouse models, increased expression of collagen X was linked with an increase in calcification, while greater expression of nucleotide pyrophosphatase phosphodiesterase (NPP1) was associated with decreased calcification.1 Then, through BCP interaction with the extracellular matrix, the LRP6 receptor is phosphorylated in the canonical Wnt pathway, which has been implicated in bone disease, leading to the differentiation of chondrocytes. Dr. Bertrand called it “a vicious cycle.”
“BCP crystals perpetuate the hypertrophic differentiation of chondrocytes,” she said. “The data suggest that OA is characterized by the reactivation of molecular signaling cascades that, at least in part, resemble endochondral ossification.”
Calcific Tendinopathy
Christelle Darrieutort-Laffite, a PhD student in rheumatology at the University of Nantes in France, said a new analysis of cadaver samples produced somewhat surprising findings on calcific tendinopathy in the rotator cuff that shed light on the nature of the disease, but also raise other questions. This is a common disease, Dr. Darrieutort-Laffite said, but its origin is still mostly unexplained, with the molecular and cellular mechanisms not well identified.2
In the study, researchers collected samples from cadavers and used ultrasound to find calcified tendons. Then they were analyzed with micro computed tomography (CT) to assess how the deposits were distributed. Several types of histological staining were performed.
Researchers found several patterns. In two samples, small calcifications were spread between fibers in the tendons. In two others, larger deposits were encapsulated in fibrous tissue. In another, osseous changes to the tissue were seen in the tendon.
