Although rheumatologists do not know the cause of giant cell arteritis (GCA), researchers have identified many of its risk factors. These factors have largely been determined based on cohorts of patients of Northern European descent that include information about age, sex and HLA DRB1. These past studies have also suggested GCA is uncommon in black patients.
Although rheumatologists do not know the cause of giant cell arteritis (GCA), researchers have identified many of its risk factors. These factors have largely been determined based on cohorts of patients of Northern European descent that include information about age, sex and HLA DRB1. These past studies have also suggested GCA is uncommon in black patients.
New Findings
Although biopsy-proven GCA occurs more commonly in women, recent research indicates its rates are similar between races. The research by Anna M. Gruener, BMBS, an ophthalmologist from Nottingham University Hospitals National Health Service Trust, U.K., and colleagues suggests GCA does not occur more frequently in white patients than in black patients. The investigators published their findings online Aug. 8 in JAMA Ophthalmology. The retrospective cohort study compared the incidence of biopsy proven GCA in black patients with white patients.1
“In our 10-year retrospective study of GCA at the Johns Hopkins Wilmer Eye Institute, we reviewed the medical records of 586 patients who had [temporal artery biopsies], 93 of whom had positive findings,” write the authors in their discussion. “To our knowledge, the only other North American study of GCA incidence with a comparable sample size to ours evaluated patients from Olmsted County, Minn., where the population is predominantly white. That study identified 173 incident cases of GCA during a 50-year study period. Our study is the largest, to our knowledge, to examine GCA incidence in a population that includes a sizeable proportion of black patients.”
The researchers calculated an overall age- and sex-adjusted incidence rate of biopsy-proven GCA of 3.5 (95% confidence interval [CI], 2.5–4.5) per 100,000 population per year.
The Patients
The investigators evaluated patients seen at the Johns Hopkins Wilmer Eye Institute, Baltimore. Patients were selected for temporal artery biopsies based on their clinical presentation. Although the population in the current study differed from previous studies with regards to ethnicity, it was similar to previous studies in terms of mean age (70.5 years) and sex ratios (72.2% women). The mean age of patients selected for temporal artery biopsy was higher in 31 white patients than black patients, mean difference of 2.7 years (95% CI, 0.6–4.7 years; P=0.01).
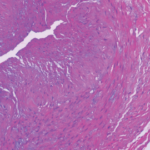
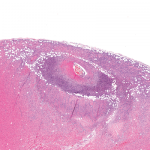
The researchers classified patients with biopsies of healed arteritis as having biopsy-proven GCA. For this classification, the healing could be a significant fragmentation and/or loss of internal elastic lamina with associated thinning and fibrosis or scarring of the media, sometimes with capillary neovascularization. The researchers classified indeterminate findings of biopsies as negative.
Thirteen patients selected for temporal artery biopsies were younger than 50. Of those patients, one black patient had a positive biopsy result. Because the concept of patients younger than 50 years old developing GCA is controversial, the researchers excluded this patient from further analysis.
The investigators found 16.1% of the 573 patients who were 50 years and older and underwent testing had biopsy-proven GCA (8.4% of black patients and 19.6% of white patients). The researchers found indeterminate results in 13 patients (two black and 11 white). The mean age of patients with biopsy-proven GCA was similar in white and black patients, with a mean difference of 1.3 years (95% CI, -3.9 to 6.7; P=0.61).
The investigators calculated that, for black patients, the crude annual incidence rate for biopsy-proven GCA was 2.9 (95% CI, 1.3–5.5) per 100,000. For white patients, it was 4.2 (95% CI, 3.0–5.6) per 100,000. When they performed a logistic regression analysis, the association between biopsy-proven GCA and white race persisted (OR, 2.5; 95% CI, 1.4–4.4; P=0.003). An adjustment for race yielded a rate per 100,000 population of 2.3 (95% CI, 1.2–3.5) for men and 4.4 (95% CI, 2.9–5.8) for women. When the researchers performed population-adjusted age- and sex-standardized incidence rates, they calculated rates of 3.1 (95% CI, 1.0–5.2) per 100,000 for black patients and 3.6 (95% CI, 2.5–4.7) per 100,000 for white patients. Although they were able to calculate an incidence rate ratio of 1.9 in women compared with men (95% CI, 1.1–3.4; P=0.03), the investigators found no significant difference between white and black patients (1.2; 95% CI, 0.6–2.4; P=0.66).
Surprising Results
“I think the results are indeed surprising,” says Sebastian Unizony, MD, co-director of the Vasculitis and Glomerulonephritis Center at Massachusetts General Hospital, Boston. “However, with [some] reports suggesting otherwise and considering that in clinical practice the great majority of the patients are white—at least in my experience—the results need to be replicated. In the meantime, rheumatologists need to be aware that GCA in African Americans may not be as rare as previously reported and keep a high index of suspicion not to miss potential cases.”
Tanaz Kermani, MD, director of the University of California, Los Angeles, Vasculitis Program agrees. She notes, “There are other diagnoses, including other forms of vasculitis, that can cause inflammation of the temporal arteries and look like GCA. Further study is needed to confirm these findings. Meanwhile, physicians should continue to evaluate anyone with symptoms that are suspicious for GCA appropriately, with studies including biopsy regardless of the race.”
Dr. Kermani points out the new study has limitations that are worth considering. Although the authors concluded the number of patients with GCA was similar in black and white populations, only 15% of the total number of patients with a positive biopsy were black. She also notes that a diagnosis of healed arteritis is controversial and stands in contrast to biopsy findings that are unequivocal or positive.
Lara C. Pullen, PhD, is a medical writer based in the Chicago area.
Reference
- Gruener AM, Poostchi A, Carey AR, et al. Association of giant cell arteritis with race. JAMA Ophthalmol. 2019 Aug 8. [Epub ahead of print]
Updated Oct. 27, 2019, to correct mistakes made in editing.