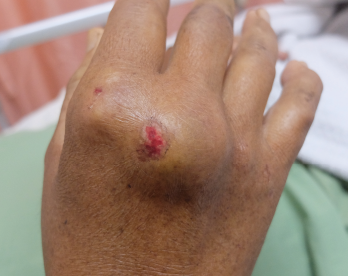
Gouty arthritis of the hand.
Casa nayafana / shutterstock.com
CHICAGO—The Gout and Hyperuricemia scientific session at the 2018 ACR/ARHP Annual Meeting opened with a talk by Tony R. Merriman, PhD, a research professor at the University of Otago, New Zealand. His talk focused on molecular epidemiology, with an emphasis on the interactions between genes and environmental exposures, and their contributions to gout.
Dr. Merriman began by explaining that although hyperuricemia (HU, the production of uric acid or urate from the liver) is the essence of gout, actual gout flares occur when the immune system responds to the uric acid crystals. HU can be exacerbated by under-excretion of urate through the kidney and gut, and is caused by a combination of inherited genetic variants and environmental exposures. Although the genetic contributors to HU are well understood, the genetic components of the immune response to gout crystals remain less well understood.
Researchers have found erosions from tophi on ancient bones in Pacific archeological sites that suggest the primitive cultures of Polynesia had a crude gout prevalence of 6%.1 Polynesians are inherently hyperuricemic and tolerate HU well when they follow their native lifestyle. As Polynesians migrated to New Zealand and encountered a Western lifestyle, however, they experienced an increased prevalence of gout, which occurred absent a substantive change in uric acid levels.2,3
Although Polynesians have a urate threshold impervious to the environment, Europeans do not. Europeans and others demonstrate a more pronounced increase in urate and gout with migration and time. This distinction means the Polynesian data cannot be used as general population-based data.
Dr. Merriman then discussed the role of diet as a cause of gout in European men.4 He explained that although the European diet has changed significantly from the 1950s until now, it appears diet alone doesn’t explain the extreme increase in urate levels. However, diet may explain gout flares. Approximately 75% of patients report dietary triggers for their flares, the most common of which are alcohol and red meat. Moreover, a case-controlled crossover study revealed that purine-rich foods can cause gout.5
The data in Polynesia and Europe are thus consistent with the finding that although diet contributes to gout, it is less of a factor in HU. In fact, urate levels appear to be 60% heritable.6 Genome-wide association studies (GWAS) have examined many millions of common genetic variants to determine which regions of the genome associate with HU or gout. These studies revealed existing and new urate transporters and, in particular, identified the gene encoding Solute Carrier Family 2 Member 9 (SLC2A9), a re-uptake transporter for urea, and the gene encoding ATP Binding Cassette Subfamily G Member 2 (ABCG2), a urea secretory transporter in the gut.7,8 A more detailed analysis of the GWAS data, however, has revealed many loci that do not contain obvious transporters, and scientists do not yet know the biology behind most of these loci.9


