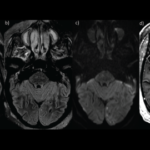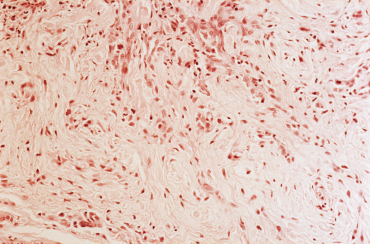
Lichen myxedematosus and scleromyxedema.
Biophoto Associates / Science Source
Scleromyxedema is a rare, mucinous skin disorder of unknown origin, one of a number of conditions that mimic systemic sclerosis. Although cases of scleromyxedema remain rare, a better understanding of its mechanisms of action could have implications for the research and treatment of scleroderma and related autoimmune conditions, says Laura K. Hummers, MD, ScM, co-director of the Scleroderma Center at Johns Hopkins University School of Medicine, Baltimore.
“We don’t know the actual prevalence of scleromyxedema, in part because rheumatologists don’t always think to look for it,” says Dr. Hummers, corresponding author of an open-label, observational report on 15 patients with scleromyxedema and the impact of intravenous immunoglobulin (IVIG) therapy published in the journal Arthritis Care & Research.1 “When I reviewed the indexed medical literature, I found a total of 200 cases referenced, mostly case reports.”
This potentially life-threatening systemic disorder is associated with profound central nervous system disturbances, including seizures and coma, and can also involve inflammatory polyarthritis, proximal myopathy and gastrointestinal abnormalities. Scleromyxedema has a similar distribution of skin findings as systemic sclerosis, with similar clinical features such as arthritis, Raynaud’s syndrome, skin fibrosis and esophageal dysmotility in some patients.
Scleromyxedema has no approved diagnostic criteria or diagnostic codes. “We don’t know the cause, although it is universally associated with monoclonal proteins. But how that connects with other aspects of the disease is not clear,” Dr. Hummers says. All but one of the 15 patients she studied had monoclonal gammopathy of undetermined significance in their blood plasma.
Franco Rongioletti, MD, chair of the Unit of Dermatology at the University of Cagliari, Italy, and colleagues have also reported on case studies of European scleromyxedema patients and progress in developing diagnostic criteria and lines of treatment.2 They found monoclonal gammopathy in 27 of 30 patients and confirmed that scleromyxedema is a chronic and unpredictable disease with severe systemic manifestations and a guarded prognosis.
Treatment Almost Always Succeeds
“What landed scleromyxedema on my plate at the Scleroderma Center is that we had seen a couple of case reports about its treatment with intravenous immunoglobulin (IVIG). Then we picked up a few patients of our own and successfully treated them with IVIG,” Dr. Hummers tells The Rheumatologist.
But immunoglobulin comes with complications, including potential for blood clotting during treatment. A bigger problem? Its high cost, up to $15,000 per treatment, initially given monthly. “We also need to infuse it very slowly. It takes two to five days, with a home healthcare nurse present, to administer a single dose,” says Dr. Hummers.