Monkey Business Images/shutterstock.com
A large medical specialty society for ophthalmologists recently updated its recommendations for the screening of chloroquine (CQ) and hydroxychloroquine (HCQ) retinopathy.1
The recommendations from the American Academy of Ophthalmology (AAO) affect patients who may use CQ or HCQ for rheumatoid arthritis or systemic lupus erythematosus (SLE), as well as some inflammatory and dermatologic conditions. The drugs are also used as anti-malarials. Retinopathy caused by these medications is not treatable, and toxicity can occur even after a patient has stopped using the agents.
The new guidelines were published in the June issue of the journal Ophthalmology.
The guidelines were last updated in 2011. The authors, led by Michael F. Marmor, MD, Department of Ophthalmology and Byers Eye Institute, Stanford University of Medicine, Palo Alto, Calif., decided to update the guidelines once again because of research published in 2014 that shed some new light on the topic.2 “The recent publication of a large demographic study has shown that toxicity is not rare among long-term uses of the drug, and the risk is highly dependent on the daily dose by weight,” the authors wrote.
In the 2014 retrospective case-control study, the records of 2,361 patients who had used HCQ continuously for at least five years were reviewed. All patients had visual field testing or spectral-domain optical coherence tomography (SD OCT) performed. The overall prevalence of HCQ retinopathy was 7.5%; with a daily consumption of 4.0 to 5.0 mg/kg, retinal toxicity prevalence remained less than 2% in the first 10 years. However, that jumped to almost 20% after 20 years of use. The study also found other major risk factors for retinal toxicity, including kidney disease and concurrent tamoxifen therapy. The research suggested that HCQ retinopathy is more common than once thought, the authors concluded.2 They also said that daily consumption of 5.0 mg/kg based on real body weight or less is associated with a low risk for up to 10 years.
The New Guidelines
Under the revised guidelines, the AAO recommends the following to clinicians for the screening and monitoring of HCQ and CQ toxicity:
- Keep the daily dosage of HCQ to 5.0 mg/kg or less of real body weight. Although there may be rare cases where higher doses are needed, clinicians should aim for a lower limit whenever possible.
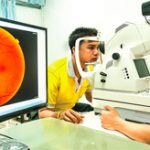
- All patients beginning long-term HCQ or CQ therapy should have a baseline eye exam in the first year of starting the drug. This helps document any complicating ocular conditions and establish a record of the fundus appearance and functional status, the authors wrote. “Most critical is fundus evaluation of the macula to rule out any underlying disease that might make use of these drugs unwise because of preexisting tissue damage or interference with the interpretation of screening tests.”
- Baseline visual fields and SD OCT are not necessary unless abnormalities are present, such as a focal macular lesion or glaucoma.
- If patients are taking the recommended dose, then annual screening is not necessary until there has been five years of exposure to HCQ or CQ. At that point, annual screenings can give ophthalmologists time to perform repeat tests or additional tests when results are suspicious.
- More frequent screenings should be considered in patients with major risk factors, such as major weight loss, kidney disease and tamoxifen use. Clinicians should always check the dosage relative to weight.
- Because there is a greater risk for toxicity beyond the macula in Asian patients, ophthalmologists should use wider test patterns (24–2 and 30–2) when performing visual fields in this patient group.
- If definitive signs of retinopathy are found, the prescribing physician should work with the patient and their ophthalmologist regarding the need to halt the medication and to ensure that any potential disease flare-ups are managed.
The authors of the guidelines said their goal is not to discourage the use of HCQ and CQ. “Screening can be viewed as a means of helping patients to continue HCQ or CQ (by not stopping the drugs for certain findings) as much as a means of preventing serious retinal damage (by the early recognition of definitive findings),” they wrote.
Rheumatologists, Ophthalmologists Weigh In
The updated guidelines seem in step with today’s practice patterns but may require some adjustments, clinicians said.