Given how unexpectedly front and center hydroxychloroquine has been in discussions about the treatment of COVID-19 this year, it makes sense to look at how it became so central to the treatment of a rheumatologic condition.
In 1991, an article appeared in The New England Journal of Medicine that would alter the way rheumatologists approached treatment for systemic lupus erythematosus: “A Randomized Study of the Effects of Withdrawing Hydroxychloroquine Sulfate in Systemic Lupus Erythematosus.”1 Although questions remained about optimal dosing, the study opened the way for much follow-up research that would confirm the drug’s critical importance for lupus patients.
Antimalarials: Background
Scientists synthesized the first antimalarial drugs shortly before the start of World War II. Malaria was a leading cause of death among soldiers, particularly in the South Pacific. The first antimalarial, quinacrine, produced numerous side effects, prompting researchers to develop derivate compounds. The U.S. Army introduced chloroquine, one of these compounds, in 1943.2
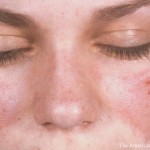
In 1951, Francis Page, MD, reported that quinacrine had beneficial effects on lupus symptoms.3 A similar report appeared two years later, when James Charles Shee, MD, published findings demonstrating that soldiers with rheumatoid arthritis (RA) or lupus taking chloroquine showed clinical improvement.4
Michelle Petri, MD, MPH, co-director of the Johns Hopkins Lupus Center and a professor of medicine at Johns Hopkins School of Medicine, Baltimore, elaborates on the discovery of the drug’s use in inflammatory conditions. “The military personnel who had rheumatoid arthritis and lupus felt much better when they were taking the malaria medicine and then wanted to continue it when they left the military,” she explains. “It’s almost a discovery made accidentally, as so many medical discoveries are. It’s a nice story of physicians listening to their patients.”
Modifications to chloroquine eventually led to the introduction of an antimalarial purported to have fewer side effects, hydroxychloroquine, which the U.S. Food & Drug Administration (FDA) approved in 1955.2 The most commonly reported adverse effects of antimalarials are mild, such as gastrointestinal discomfort or headache. However, other concerns about the safety of antimalarials emerged over time, partly because doses for rheumatological conditions were much higher than those used for malaria prophylaxis.
A population-based, case-controlled study from 2019 demonstrated that the mortality risk increased almost fourfold in people who had to stop taking their hydroxychloroquine. It is the only drug that has been demonstrated to improve the survival of lupus patients.
In the late 1950s, reports began to appear documenting retinopathy resulting from chloroquine treatment.5 This important potential adverse effect continues to influence prescribing practices to this day.
Both chloroquine and hydroxychloroquine can potentially bind in the retinal pigment epithelium and cause degeneration of photoreceptors, leading to retinopathy.6 Eventually, research demonstrated that hydroxychloroquine posed less of a risk of retinopathy than chloroquine.
In the U.S. and Canada, hydroxychloroquine has largely replaced chloroquine as a treatment for lupus in the antimalarial drug class.