
When rheumatologists and social workers collaborate, patients benefit.
Monkey Business Images/shutterstock.com
At the Hospital for Special Surgery (HSS), New York, rheumatologists and social workers have found that an interdisciplinary approach to care for systemic lupus erythematosus (SLE) patients improves the overall patient experience.
“Our goal is to help patients navigate the complex healthcare system,” says Jillian Rose, LCSW, MPH, assistant director, Community Engagement, Diversity & Research. “We help patients co-create a solid care plan that suits their needs and lifestyle. Even though their illness may be out of control, we want patients to feel more in control and at the center of their care.”
The HSS offers more lupus support and educational programs than any other hospital in the U.S. These programs are an integral part of the Department of Social Work Programs and work in close partnership with the Lupus and Antiphospholipid (APS) Center of Excellence at HSS. The center was established to provide individualized, state-of-the-art care, support and education to patients with lupus and APS.
“Our close relationship with social workers makes these goals achievable,” says Jane Salmon, MD, rheumatologist and director of the center. Patients are given access to expert physicians, social workers, research studies, nursing services and educational programs.

Ms. Rose
New SLE patients meet with a social worker to assess their emotional concerns and practical needs. Rheumatologists actively refer patients to support programs, knowing that individuals with SLE can be confronted by many psycho-social issues.
“We build programs around patients’ needs, which are determined by frequent needs assessments and what is important to them,” Ms. Rose says. “Culturally tailored programs in English, Spanish and Chinese target patients in different communities.”
“Going to HSS is the best resource that I have,” says Ivette Salmon, a 59-year-old lupus patient from Queens, N.Y. “Sometimes, I blame everything on my lupus, but I’ve learned that issues can also arise from other conditions caused by lupus. It’s helpful to talk about challenges with someone who has faced the same problems.”

Dr. Salmon
Given the broad range of issues that arise in the care of these patients, social workers also attend appointments with lupus patients on a case-by-case basis and at the patient’s request. “Social workers will articulate any issues the patient has expressed, such as the inability to pay for prescriptions, which can be challenging for patients to bring up on their own,” Ms. Rose says. “While a physician may not think a $10 co-pay for a medication is significant, for some patients it is. Factors such as a patient’s inability to pay for medicines or difficulty getting transportation can lead to adherence issues and can derail their treatment plan.”
Here’s a closer look at the center’s offerings:
Lupus Center of Excellence Weekly Clinic Conference
This weekly conference embraces a multidisciplinary team approach to manage complex patients and creates a unique training environment for rheumatology fellows. Residents, fellows, rheumatology attendings and other medical specialists (e.g., dermatologists, nephrologists, psychiatrists), study coordinators and social workers meet to discuss SLE patients seen in the clinic.
“Contributions from all of these disciplines allow us to implement the best program of care tailored for each patient,” Dr. Salmon says. In addition, “Issues of compliance, trust in the healthcare provider, lack of housing and inability to pay for care are discussed.”
Because a healthcare team’s beliefs, values, attitudes and judgments can sometimes conflict with those of the patient, a social work manager along with clinic staff use consultative practices to assess each patient’s concerns related to the impact of lupus, choice of treatments, psychosocial status and present active issues during the conference to guide physicians’ decisions. “Social workers assess patient barriers related to culture, mental health, treatment adherence, insurance status, language and education and help the team develop approaches to overcome impediments,” Dr. Salmon says.
SLE Workshops, Including Lupus Research Presentations
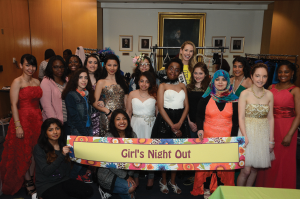
HSS partnered with Project Sunshine to hold the annual Charla de Lupus Girls Night Out/Parents Spa Day on April 7, 2016, for young women with lupus and their parents and caregivers. During the event, which was hosted by the Charla de Lupus (Lupus Chat) Program at HSS, about 20 patients enjoyed a night of fun picking out prom dresses and getting their hair and makeup done. Miss USA 2015, Olivia Jordan, joined HSS and Project Sunshine staff to help the girls.
Photo courtesy of Hospital for Special Surgery.
Monthly presentations on topics of interest to patients are followed by a support group session. For example, during a presentation about lupus research, attendees learned about HSS’ innovative studies to understand their disease or test new treatments. “Patients gain an understanding of the different types of studies (e.g., clinical trials vs. registries) and can determine which, if any, are right for them to explore eligibility and participate in,” Dr. Salmon says. “Guided by social workers, and in the presence of basic and clinical investigators, patients ask questions and share their experiences. This forum has the potential to empower patients to help themselves and participate in research studies.
“Similarly, programs about sun protection, nutrition and reproductive health stimulate discussion among patients and provide a more trusted environment to educate them.”
Charla de Lupus (Lupus Chat)
This program reaches underserved communities and provides health support and education via a bilingual national telephone line and at four hospital clinics throughout New York City. “From our needs assessment, we found a gap in reaching minorities and younger patients (ages 13 to 35),” Ms. Rose says.
“Dialogues between physicians caring for SLE patients and social workers who lead the program identify key patient needs and provide information which can be conveyed to patients by peers, so it is more easily accepted,” Dr. Salmon says. For example, a focus on increasing access to high-quality reproductive health counseling and care may decrease the frequency of serious pregnancy complications associated with becoming pregnant when SLE disease activity is not well controlled.
Social workers provide support to patients who are managing anxiety and cultural issues. By serving as a buffer, they can help increase trust and adherence between patients and their care team. For example, a patient may be hesitant to tell their rheumatologist that they are supplementing their treatment program with herbs. “But it’s important to share that with their doctor, because there could be an interaction,” Ms. Rose says.
The program also hosts special events in which HSS staff can become better acquainted with patients and their families. “This helps to build trust and makes patients feel more comfortable about opening up about their barriers to adherence,” Ms. Rose says.
Social workers provide support to patients who are managing anxiety & cultural issues. By serving as a buffer, they can help increase trust & adherence between patients & their care team.
LANtern (Lupus Asian Network)
Dr. Salmon examines a patient.
This may be the only national, hospital-based support and education program dedicated to serving Asian Americans with lupus and their families. “Perceptions about lupus being fatal, societal stigma, language and cultural beliefs, and traditions should be considered when implementing a care plan to avoid barriers and challenges to care,” Dr. Salmon says.
The social work senior manager who leads LANtern provides specifically tailored community programs for Asian lupus patients, and they collaborate with other healthcare professionals and community organizations to enhance awareness, empower patients and provide support and tools to patients and their families to better manage the disease.
LupusLine
This free telephone counseling service provides one-to-one support for people with lupus. It is the only national, hospital-based telephone peer support program that links people who are referred to the service with trained volunteers who have lupus. “Veteran peer counselors are supervised by a social work manager,” Dr. Salmon says. “Patients learn from others with the condition in a way that they cannot learn from their healthcare professionals.”
“The program’s success depends upon the social worker’s ability to closely match patients with particular concerns with counselors who may have had those same medical or social life experiences,” Ms. Rose says. “A peer counselor can help normalize a situation.” The program has now expanded globally via the Internet.
Teen & Parent Lupus Chat Groups
Monthly in-person chat groups for teens and their parents provide a place to discuss lupus-related issues and identify with their peers. For parents, it provides a community for managing the illness’ unpredictability.
“Fun activities, such as prom night, help patients forget about lupus for an evening,” Ms. Rose says. “Designers donate dresses and teens get glammed up. Their physician becomes their personal shopper for the day, and patients see that their doctor is human, too.”
Lupus Steering Committee
A steering committee comprising a team of rheumatologists who specialize in SLE and APS management, physician–scientists who study these diseases, nurses and social workers meets monthly to evaluate and expand the center’s programs.
“We review ongoing research projects, patient educational programs and community engagement events,” Dr. Salmon says. “We fund pilot grants in SLE and APS by HSS staff and trainees, discuss and suggest treatment guidelines for specific manifestations of SLE and develop quality initiatives to monitor our delivery of general and lupus-specific medical care. Social work team members are invaluable for projects related to patient-reported outcomes, patient educational programs and community outreach activities.”
Final Thoughts
Rheumatologists and social workers at HSS, in collaboration with patients, have developed unique interdisciplinary, evidence-based strategies to achieve better outcomes in managing the care of SLE patients. In fact, some of their programs are one-of-a-kind in the nation.
By offering a variety of patient-centered and culturally tailored services, healthcare providers at HSS believe they are helping SLE patients to deal with the many challenges they face.
Karen Appold is a medical writer in Pennsylvania.
Interdisciplinary Research Initiatives
As part of their interdisciplinary approach to improve care for systemic lupus erythematosus (SLE) patients, rheumatologists and social workers at Hospital for Special Surgery (HSS) work together to conduct research that benefits these patients.
For example, staff from the two disciplines have co-authored and presented abstracts at conferences about the impact of their joint care from both the medical and psychosocial perspectives. “We’ve published about HSS’ SLE programs and about issues that concern both rheumatologists and social workers,” says Jillian Rose, LCSW, MPH, assistant director, Community Engagement, Diversity & Research.
A current project is to create a mobile health (mHealth) application (app) to help patients better manage challenges related to having lupus. “To develop the app, a rheumatologist worked with the social work team to conduct a series of focus groups in which SLE patients discussed what would help them provide better care for themselves and what they saw as their greatest challenges,” says Jane Salmon, MD, a rheumatologist at HSS and director of the Lupus and Antiphospholipid (APS) Center of Excellence. Questions explored challenges due to having SLE, current coping strategies, how an SLE app could help with disease self-management, app format and design, and priorities for app content.1 Ninety-eight percent of participants said they would use an app to help manage lupus.1
The lupus app will help patients better manage their disease by sending alerts regarding appointments and medication refills; providing education on drug interactions; providing nutrition and exercise tips; notifying them about new medications; and offering resources to cope with the emotional and psychological issues related to lupus. The app could also help patients track symptoms by having the ability to photograph a rash and send it to a physician, for example.
A second series of focus groups will be to ask SLE patients to identify important outcomes, and what barriers exist to achieving them and what enablers help to achieve them, as well as patients’ views of how healthcare providers can facilitate achievement of these outcomes.
Lupus’ Effect on Pregnancy
Another research effort focuses on pregnant women who have lupus. These women have higher rates of preeclampsia, fetal and neonatal death and fetal growth restriction. “Only a subset of lupus pregnancies end poorly, but identifying women destined for these complications remains challenging and limits our ability to counsel and care for pregnant lupus patients,” says Dr. Salmon, who led a prospective multicenter observational study, called the PROMISSE study, to identify markers that predict poor pregnancy outcome in APS and/or SLE patients.2
“We identified a panel of clinical and laboratory variables that, in the first months, can be used to anticipate outcomes of pregnancy. In addition, we identified pathways of injury to the placenta and developing fetus that provide new targets for prevention and treatment,” Dr. Salmon says.2 “Explaining to patients that fewer than 20% of pregnancies in patients with SLE or APL end with adverse outcomes, and that in the absence of specific markers, complication rates are similar to those in healthy women, helps ease their concerns.3
“And for those women with SLE who have the highest risk for preeclampsia and severe complications, we are embarking upon an interventional clinical trial with a biologic therapy to prevent these outcomes,” Dr. Salmon continues.
PROMISSE research coordinators are an important source of support to pregnant patients with lupus. They not only meet the patients at HSS during their rheumatology appointments, but they also attend monthly obstetric appointments, allowing them to develop partnerships for advocacy and support.
“Social workers collaborate closely with our research coordinators and often serve as a touch point to explore concerns in greater depth and to refer patients for peer support to other lupus patients who have gone through similar experiences,” Dr. Salmon says.4
References
- Levine AB, Batterman A, Bykerk V, et al. Patient preferences for the development of a mobile health (mHealth) application (App) for systemic lupus erythematosus (SLE) patients: A qualitative study [abstract]. Arthritis Rheumatol. 2015;67(suppl 10).
- Kim YM, Buyon JP, Guerra MM, et al. Angiogenic factor imbalance early in pregnancy predicts adverse outcomes in patients with lupus and antiphospholipid antibodies: Results of the PROMISSE study. Am J Obstet Gynecol. 2016 Jan;214(1):108.e1–108.e14. doi:10.1016/j.ajog.2015.09.066. Epub 2015 Sep 29.
- Buyon JP, Kim YM, Guerra MM, et al. Predictors of pregnancy outcome in a prospective, multiethnic cohort of lupus patients. Ann Intern Med. 2015 Aug 4;163(3):153–163.
- Kim S, Persad P, Erka D, et al. Research studies and their implication for social work practice in a multidisciplinary center for lupus care. Soc Work Health Care. 2015;51(7). doi: 10.1080/00981389.2012.683711
Editor’s note: ACR Resources
The ACR’s Lupus Initiative offers a wide range of resources for providers, patients, educators and students.


