HelloRF Zcooll / shutterstock.com
A confluence of advances in knowledge and technology is closing in on the day when therapies for patients with rheumatoid arthritis (RA) may be specifically targeted to the precise variant and stage of disease.
“Precision medicine is in the future, and not the distant future but more in the immediate future,” says Harris R. Perlman, PhD, chief of rheumatology, Department of Medicine, Northwestern University Feinberg School of Medicine, Northwestern, Ill. “I do believe we will be able to really define treatments for patients.”
For Dr. Perlman, the ability to precisely tailor treatment for patients with RA should be no different than what is already being achieved in oncology. Identification of biomarkers to help predict an individual patient’s sensitivity or resistance to a particular therapy is the future of medicine, and as in oncology, Dr. Perlman sees this as the hopeful future for patients with rheumatologic conditions, such as RA.
As in oncology, targeted treatment starts with looking at the tissue where disease is active. Oncologists biopsy tumors to find out what is going on, says Dr. Perlman, whereas rheumatologists, for many years, have relied on blood analysis to try to determine disease progression and treatment effectiveness for such diseases as RA and have not directly examined the tissue source of disease.
As knowledge about the tissues and cells involved with RA has emerged and new technologies to study these tissues have proved possible, rheumatologists are now, similar to oncologists, going directly to the tissue source to better understand the precise disease mechanisms of RA and how to better target therapies.
As in oncology, targeted treatment starts with looking at the tissue where disease is active.
Tissue Source: Synovial Biopsies
Building on research showing the importance of synovial macrophages in the pathogenesis of RA and responsiveness to treatments, Perlman and colleagues undertook a multicenter study to better understand how these cells actually work in RA. In particular, the study looked at the feasibility of using ultrasound-guided technology to collect synovial biopsies from patients with RA for histologic analysis and genetic profiling.

Dr. Perlman
Although ultrasound-guided technology to collect synovial biopsies from patients with RA has been used successfully in Europe for nearly six years, this is the first study in the U.S. to use this technology for synovial biopsy of an affected joint in a patient with RA.
The multicenter study was conducted by a consortium of six academic rheumatology groups who formed a network called the Rheumatoid Arthritis Synovial Tissue Network (REASON). All members in the consortium were trained in minimally invasive ultrasound-guided synovial biopsy techniques.
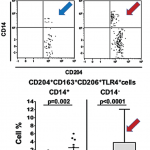
A total of 41 adult patients with RA were included in the study. Synovial biopsies obtained from all patients underwent histologic analysis, fluorescence-activated cell sorting, and genetic analysis by RNA sequencing. Specifically, the investigators looked at macrophages within the synovial biopsies by removing the macrophages from each biopsy using fluorescence-activated cell sorting and then performing RNA sequencing on the macrophage population.
“By doing that, we were able to uncover at least six populations of RA patients,” explains Dr. Perlman. Within these populations, the investigators found six different transcriptional profiles they called modules. “Each one [module] is associated with a different aspect of clinical disease,” says Dr. Perlman. For example, some modules were negatively correlated with tumor necrosis factor (TNF), some were positively correlated with methotrexate, some were correlated with early disease, and some correlated with swollen joint counts.
Proof of Principle
What the study shows is the feasibility of removing synovial tissue from patients with active RA, separating out macrophages from that tissue into individual populations and correlating their genomic profile with disease.
“All the major questions you have to ask to see if this will work have been answered,” says Dr. Perlman, emphasizing the next big step is to conduct a large study to begin to assess which patients, based on their genetic signature, will have the best response to a particular drug.
The consortium is currently working on a National Institutes of Health (NIH) grant to study this. The investigators hope to include 300 adult patients with RA in the study, take a single biopsy of each patient right when they change therapy and then watch the patient over the course of 12 weeks. The hope is to be able to determine what type of treatment works best based on a patient’s genetic profile.
If this works, both patients and society as a whole will benefit. Despite the great advances in outcomes with biologic drugs to treat RA, the response rate remains about 50%, with about 20% of patients who don’t respond to any treatment.
“The problem is that we don’t know who is going to respond or not,” says Dr. Perlman. “We waste about $2 billion a year on biologic drugs, because we don’t know which patients should get which one.”
What is needed, he emphasizes, is a system to predict which patients will respond to which drugs.
Mary Beth Nierengarten is a freelance medical journalist based in Minneapolis.
References
- Mandelin AM 2nd, Homan PJ, Shaffer AM, et al. Transcriptional profiling of synovial macrophages using minimally invasive ultrasound-guided synovial biopsies in rheumatoid arthritis. Arthritis Rheumatol. 2018 Jun;70(6):841–854.