
Studio_G / shutterstock.com
The evaluation and management (E/M) code set in the American Medical Association’s Current Procedural Terminology (CPT) book lists descriptors, as well as typical times for patient visits. These times are averages of how long it takes a physician to complete all components of a visit at each level. Because the specific times identified in the CPT book are averages, they represent a range of times that may be higher or lower depending on actual clinical circumstances from visit to visit. It’s important to understand that time is only a contributing factor in determining which level of E/M to report.
The key components of history, examination and medical decision making are usually used to determine an E/M level of service, if a provider ends up spending more than 50% of the total visit counseling and coordinating care, then time can be used as the key factor in determining the E/M level to bill for that service. Per the CPT, typical times for new and established office visits are:
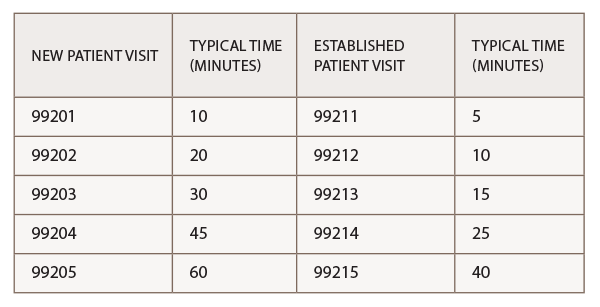
When coding on the basis of time in the outpatient setting, providers can count only face-to-face time with the patient or family. This face-to-face time includes not only the time spent counseling, but also the time associated with any history, exam or medical decision making performed. Time spent reviewing records, talking with other providers and documenting the encounter without the patient or family present cannot be considered. It is not unusual for rheumatologists to spend significant time during an office visit reviewing new and/or existing problems, modifying medications, counseling and coordinating care. To determine whether to code for time as the key factor, the following questions must be answered:
- How much time did I spend either counseling or coordinating care for the patient?
- How much time did I spend in total for the visit (including time spent providing key components and time spent counseling and/or coordinating care)?
Example
A 62-year-old male patient returns to the office for a follow-up visit for his gout. The history of present illness is extended, an expanded problem focus examination is conducted, and medical decision making is of low complexity, which would normally be coded as a level 3 visit (99213). But the total time for the visit is 30 minutes, and more than 50% of that time is spent on counseling the patient on a diet and exercise plan.
Because time and the discussion were documented and more than 50% of the visit was spent with the patient face to face, time is the key factor in determining the level of this visit. CPT states that an established patient level 4 visit is typically 25 minutes long; this visit was 30 minutes long, which qualifies the visit to be coded 99214.
In every case, it’s imperative to document the extent of the counseling/coordination of care in the patient’s medical record.

