Albina Glisic / shutterstock.com
SAN DIEGO—At two sports medicine talks at the 2017 ACR/ARHP 2017 Annual Meeting last November, two rheumatologists discussed shoulder impingement and low back pain. First, Andrew Concoff, MD, a rheumatology and sports medicine specialist at St. Jude Medical Center in Fullerton, Calif., gave these five shoulder impingement tips:
- Physical exams may not be very useful because many of them can indicate multiple shoulder conditions. The Neer test, for example, can point to supraspinatus tendinopathy, a full-thickness supraspinatus tear or subacromial impingement.
- Clinicians must learn whether an injury was macrotrauma (e.g., a sudden major injury of some kind) or microtrauma (e.g., the cumulative effect of smaller motions). Also important is whether the injury is to the dominant shoulder, because patients can tolerate an injury on their nondominant side easier than their dominant side, and because rotator cuff tear repairs tend to perform better on the dominant side. Clinicians also must know their patient’s demands: Will they engage in a lot of potentially problematic overhead activity, for example, or in such activities as bowling or gardening, which people can tolerate well even with major rotator cuff tears?
- Scapular dyskinesis (SD), or abnormal shoulder movement, is best handled with physical therapy (PT) that targets SD. “If we focus on stabilizing the scapula, we can actually improve things to such an extent that even five years later, with the same program, [patients] randomized to specific scapular exercises continue to not want surgery,” he said.1
- Studies have found no difference in outcomes between operative and non-operative approaches to symptomatic, atraumatic, full-thickness rotator cuff tear, so initial PT seems appropriate, Dr. Concoff said. “This is why I like to know up front if somebody has or doesn’t have a rotator cuff tear, and then I like to know if it’s traumatic or not,” he said.
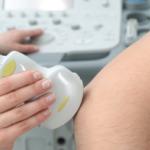
- Ultrasound provides good, positive predictive value for full-thickness rotator cuff tear, similar to that of MRI. Plus, it costs less than MRI, patients prefer it over MRI and it also allows better injection accuracy and outcomes. “Ultrasound works very well in this scenario,” he said. Leveraging ultrasound in this manner represents one piece in a larger effort toward “value-driven redesign” of both orthopedic and rheumatologic musculoskeletal care.
Low Back Pain
In another sports medicine talk, Jean Gillies, MD, a clinical instructor of rheumatology at the University of British Columbia in Vancouver, discussed the need for a better approach to low back pain. Too often, she said, it’s simply called “nonspecific low back pain,” which doesn’t help clinicians determine a treatment course, she said.