New Africa / shutterstock.com
ATLANTA—Two ways to investigate injuries to the upper extremities are by in-depth physical examinations and ultrasound. In a Clinical Practice session at the 2019 ACR/ARP Annual Meeting, Anatomy: Correlating Physical Exam and Ultrasound in Common Sports Injuries of the Upper Extremity, Carlin Senter, MD, FACP, associate professor of primary care sports medicine at the University of California, San Francisco, and Anthony M. Reginato, MD, PhD, associate professor and director of the Division of Rheumatology at Brown University, Providence, R.I., presented strategies to diagnose different injuries via case studies.
Most sports medicine problems can be identified by conducting a careful history and physical exam and knowing your anatomy, said Dr. Senter. “However, musculoskeletal ultrasound is playing an increasingly important role in both diagnosis and guiding treatment for sports medicine problems.”
In the session, Dr. Reginato reviewed basic principles of ultrasound. An ultrasound transducer converts electrical energy into acoustic pulses (i.e., sound) and transmits them into the body. Through the piezoelectric effect (generation of an electric charge in response to applied mechanical stress) the transducer acts as a receiver of refracted echoes and converts them into electrical signals, which are finally processed as an image.
Going Gray
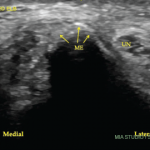
The content of various tissues will differentially reflect the transmitted pulses, resulting in different gray images. Hyperechoic structures (white on the screen) are those with an increased density of sound waves compared with surrounding structures, such as bone, tendon, nerves and calcification. Hypoechoic structures (gray on the screen), including the synovium, lymph nodes and some tumors, give off fewer echoes. Anechoic structures, appearing black on the screen, are those without an echo, such as fluid and cartilage.
‘Musculoskeletal ultrasound is playing an increasingly important role in both diagnosis & guiding treatment for sports medicine problems.’ —Carlin Senter, MD, FACP
“In rheumatology, ultrasound can predict diagnosis—as well as provide early detection—staging of the disease and monitor response to therapy,” said Dr. Reginato.
A Case of Shoulder Pain
In one case, a 57-year-old man presented with right shoulder pain that started after he had slipped and fallen three months earlier. He tried physical therapy without benefit and was waking up at night due to pain. On physical exam, the shoulder was not tender. The active range of motion of the shoulder was intact, with pain on abduction between 60º and 120º. He had moderate pain with resisted external rotation of the shoulder and was unable to perform a lift-off test. The diagnosis was a rotator cuff tendon tear.