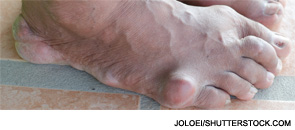
The concept of difficult-to-control gout describes several clinical head-bangers.
It may refer to failure to achieve the recognized target serum urate level of <6.0 mg/dL despite adequate therapeutic efforts with urate-lowering agents. It can refer to failure to suppress or stop gout flares, or it can describe failure to prevent the disease progression. All too often, all three collide.
The Stumbling Blocks
The causes of difficult-to-control gout fall on the shoulders of both patients and the medical professionals caring for them.
On the patient side, previous negative experiences with gout therapies; nonadherence to complex treatment plans; and unwillingness to curtail behavioral patterns, such as daily beer drinking, often compound a poor understanding of which medication is used for which feature of gout.
Many gout flares are seen in emergency departments or primary care practices where clinicians are often unaware of best practices in gout management when comorbidities feature strongly. They frequently fail to make the diagnosis, may trivialize intermittent flares and are often late to initiate urate-lowering therapy. Often, they lack the time to embrace a high-intensity approach, which is usually needed to control the hyperuricemia and gout. Treating to a serum-urate target is not yet well integrated into primary care practice. The concept of providing antiinflammatory coverage to mitigate flares following the initiation of urate-lowering therapy is still new to many.
There is a widespread failure of both patients and clinicians to understand contemporary gout treatments. Newly published guidelines do articulate the distinct goals of urate-lowering therapy, gout flare prophylaxis and acute flare pain control, but a big disconnect remains between the guidelines and clinical practice.
Many patients with hyperuricemia and gout are perceived as being too complex to treat effectively. However, it’s just those patents who should be referred for rheumatologic care.
This case highlights many of the challenges facing patients and clinicians.
The Case
EH was a 60-year-old white man with a 10-year history of gout, which first manifested as episodic, acute-onset flares of monoarthritis in the lower extremities with pain and swelling. These typically lasted four to seven days. He would try to self-medicate using acetaminophen or low doses of nonsteroidal antiinflammatory drugs (NSAIDs). When this approach failed to alleviate his symptoms, he would go to an emergency department. He never discussed these events with his primary care physician, whom he saw infrequently.
Five years ago, he was referred to our rheumatology clinic by our emergency department after an especially long flare, his third gouty attack that year.


