Although varicella zoster virus may play a role in the pathogenesis of giant cell arteritis (GCA), research suggesting that reactivation of the varicella zoster virus is an infectious trigger of GCA has been difficult to replicate.1 Further, some physicians have expressed concern that treating GCA patients with antivirals based on this assumption may have negative effects on patients’ overall health. This approach may not effectively treat GCA, according to Robert Padera Jr., MD, PhD, a pathologist at Brigham and Women’s Hospital, Boston.
Dr. Padera and his rheumatologist and pathologist colleagues have sought to better understand the potential association between the varicella zoster virus and GCA development. “The field has learned much about the downstream steps in the pathogenesis of GCA, including the role of dendritic cells and inflammatory cell recruitment, but the initial activating event remains unclear,” he says.
Testing for a Connection
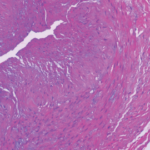
Together, Dr. Padera and his team designed a study to detect the presence of the virus in temporal artery biopsies and ascending aortic resections that were immunostained using a combination of varicella zoster virus antibodies. The researchers identified 41 temporal artery biopsies and 47 ascending aortic resections that were positive for GCA from 2007–2017. Each test specimen was negative for varicella zoster virus by morphology and immunohistochemistry.
An important aspect of this research involves how the test specimens reacted to the varicella zoster virus immunostain. “True staining for varicella zoster virus is strongly positive within the nucleus and cytoplasm of infected cells, with little staining of the extracellular matrix,” Dr. Padera writes in the study, published in the December 2019 issue of The Journal of Rheumatology.2
Dr. Padera further explains the interpretation of previous similar research detecting varicella zoster virus in immunostained GCA biopsies has issues because the reported areas of virus positivity in the stain don’t conform anatomically to the outline of cells or other intrinsic tissue structures.1 Additionally, he suggests the difference in antibodies or immunohistochemical protocols used in the previous research may be a reason for discordance with the current findings. The prior study used an antibody recommended for use on Western blots and immunofluorescence on fresh frozen tissue, not on formalin-fixed, paraffin-embedded tissue. This difference may have resulted in false positive staining in that study.
“Our study results finding a lack of association between varicella zoster virus and GCA provide further evidence to research identifying similar results, including two recent studies that reached the same conclusion we did,” Dr. Padera says.3,4