 ACR Convergence 2021—The past year has been an exciting time for researchers and clinicians focused on the topic of connective tissue disease-associated interstitial lung disease (CTD-ILD), with advances in our understanding of these disorders and newly approved medications for their treatment. At the ACR Convergence 2021 annual Review Course, Kristin Highland, MD, MSCR, director of the Rheumatic Lung Disease Program at the Cleveland Clinic, provided an exceptional overview of this topic and future developments to expect in the field.
ACR Convergence 2021—The past year has been an exciting time for researchers and clinicians focused on the topic of connective tissue disease-associated interstitial lung disease (CTD-ILD), with advances in our understanding of these disorders and newly approved medications for their treatment. At the ACR Convergence 2021 annual Review Course, Kristin Highland, MD, MSCR, director of the Rheumatic Lung Disease Program at the Cleveland Clinic, provided an exceptional overview of this topic and future developments to expect in the field.
Significant Source of Morbidity & Mortality

Dr. Highland
Dr. Highland began by noting that CTD-ILD can be prevalent in certain rheumatic diseases and can represent a significant source of morbidity and mortality. In scleroderma, autopsy studies have demonstrated the presence of ILD in 75–95% of patients and, although scleroderma renal crisis was the leading cause of death in patients in the early 1970s, pulmonary fibrosis became the leading cause of mortality in patients with scleroderma by the early 2000s.1
In patients with rheumatoid arthritis, the prevalence of ILD is estimated to be 5–58%, with a 7.7% lifetime risk of developing this condition, which can precede articular disease in up to 20% of patients and is responsible for 10–20% of deaths.2,3
Radiographic Pattern of Disease
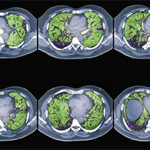
Once ILD has been identified in a patient, Dr. Highland explained that it is important to understand the radiographic pattern of disease to predict prognosis. Nonspecific interstitial pneumonia combines reticulations and ground glass opacities that tend to be peripheral with an apical to basilar gradient. This is the most common pattern of ILD seen in connective tissue diseases. The presence of ground glass opacities implies inflammatory changes that are potentially reversible. Such findings may also be seen with organizing pneumonia, particularly in patients with rheumatoid arthritis, lupus and idiopathic inflammatory myopathies.
In contrast, lymphocytic interstitial pneumonitis, most often seen in patients with Sjögren’s syndrome, and interstitial pneumonia, which can be seen in patients with idiopathic pulmonary fibrosis and rheumatoid arthritis, are fibrotic conditions that are not typically reversible with immunosuppression.
Dr. Highland showed that by combining knowledge of the pattern of ILD seen on high-resolution computed tomography (CT) imaging, the forced vital capacity (FVC) as determined by pulmonary function testing and the histopathologic pattern of disease seen on lung biopsy, patients can be grouped into subsets of CTD-ILD and survival rates can be predicted with reasonable accuracy.