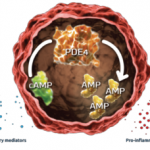
 Apremilast, a phosphodiesterase 4 inhibitor, is already approved to treat patients with psoriatic arthritis (PsA) and continues to be studied in different populations and at different doses.1 A recent study by Christopher J. Edwards, BSc, MBBS, MD, FRCP, associate director of the Southampton NIHR Wellcome Trust Clinical Research Facility, University Hospital Southampton in the UK, and colleagues evaluated the safety and efficacy of apremilast in treating patients with active psoriatic arthritis (PsA) and current skin involvement, despite treatment with conventional disease-modifying anti-rheumatic drugs (DMARDs) and/or biologic DMARDs.2
Apremilast, a phosphodiesterase 4 inhibitor, is already approved to treat patients with psoriatic arthritis (PsA) and continues to be studied in different populations and at different doses.1 A recent study by Christopher J. Edwards, BSc, MBBS, MD, FRCP, associate director of the Southampton NIHR Wellcome Trust Clinical Research Facility, University Hospital Southampton in the UK, and colleagues evaluated the safety and efficacy of apremilast in treating patients with active psoriatic arthritis (PsA) and current skin involvement, despite treatment with conventional disease-modifying anti-rheumatic drugs (DMARDs) and/or biologic DMARDs.2
This study, known as PALACE 3 (Psoriatic Arthritis Long-term Assessment of Clinical Efficacy), screened 612 patients and enrolled in the study 505 adults with PsA for six or more months who also met the Classification Criteria for Psoriatic Arthritis (CASPAR) at screening and had at least three swollen and tender joints. Patients were randomized to receive 20 mg apremilast twice daily, 30 mg apremilast twice daily or placebo. If placebo-treated patients did not achieve a 20% improvement in swollen and tender joint counts by Week 16, they received apremilast rescue treatment. At Week 24, the remaining placebo patients were then randomized to receive either 20 mg or 30 mg apremilast twice daily.
Safety and efficacy were assessed throughout the 52-week study. The ACR20 response was the primary efficacy endpoint. At Week 16, it was achieved in significantly more patients who received 30 mg apremilast twice daily and those who received 20 mg apremilast twice daily compared with placebo-treated patients (41%, 28% and 18%, respectively; P<0.0001). The mean decrease in the Health Assessment Questionnaire Disability Index (HAQ-DI) score was a key secondary endpoint. The HAQ-DI was achieved in a significantly greater number of patients treated with 30 mg apremilast twice daily compared with placebo-treated patients. At Week 16, 41% of patients treated with 30 mg apremilast achieved PASI-50 compared with 24% of placebo-treated patients. This result was statistically significant. For the 20-mg-apremilast-treated patients at Week 16, 33% achieved PASI-50—which was numerically higher, but not statistically significant.
Additionally, at Week 16, significantly more patients treated with 20 mg or 30 mg apremilast achieved PASI-75 compared with placebo-treated patients (20%, 21% and 8%, respectively).
In patients who continued therapy, sustained efficacy was demonstrated at Week 52. Most adverse events were mild to moderate in severity, the most common of which were diarrhea, headache, nausea and upper respiratory tract infection.
Michele B. Kaufman, PharmD, CGP, RPh, is a freelance medical writer based in New York City and a pharmacist at New York Presbyterian Lower Manhattan Hospital.