- Antibodies to Yo/CDR2 antigen in paraneoplastic cerebellar degeneration, which are associated with breast and ovarian cancers;
- Antibodies against Ri/NOVA (neuro-oncological ventral antigen) in paraneoplastic opsoclonus-myoclonus ataxia in those with small cell lung, breast and ovarian cancers; and
- Antibodies against TIF-1-gamma (p155/140 antibody), which are hypothesized to be overexpressed in certain malignancies.
Why Should We Care?
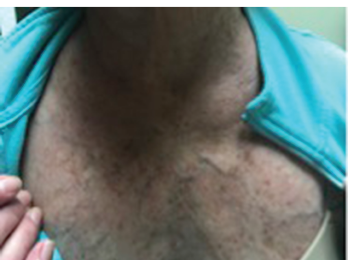
Figure 3: The flushing rash of carcinoid can mimic the rash of dermatomyositis, particularly the V sign, which refers to macular erythema over the anterior neck and upper chest.
P155/140 antibodies, which target transcriptional nuclear factor TIF-1-gamma, were first described by Targoff et al.7 It is of interest because it could potentially predict which dermatomyosits patients have an underlying malignancy. Prior to this, it was noted the presence of other myositis-specific antibodies decreased the likelihood of concurrent malignancy. Kaji, et al. further confirmed this, but their sample sizes were small.8 Later on, Chinoy et al. analyzed a large cohort of inflammatory myopathy patients and found anti-155/140 is dermatomyositis specific, and out of the 16 cancer-associated myositis patients, eight were positive for this antibody, implying 50% sensitivity and 100% specificity.9
Screening for malignancies in dermatomyositis patients
Although it’s generally accepted dermatomyositis patients should be screened for cancer, no consensus exists as to what screening should entail. Experts have suggested blind testing is not helpful, while others say CT scans and gastrointestinal endoscopy may play a useful role.
In the largest study to date, two large dermatology cohorts were used to identify 400 patients with dermatomyositis.10 In this study, 15.8% of patients had cancer, 72% occurring within five years of dermatomyositis-symptom onset, suggesting a temporal component. In descending order, the most frequent types of cancer were breast, hematologic and colorectal. The vast majority of the cancers (42%) were diagnosed after the dermatomyositis diagnosis and were associated with suspicious signs, such as unintentional weight loss, melena or persistent abdominal pain. It seems reasonable to screen all patients with dermatomyositis for malignancy using age-appropriate guidelines.
The difference between carcinoid & dermatomyositis skin manifestations
Several hallmark skin manifestations of dermatomyositis exist. Gottron’s papules are lesions consisting of erythematous to violaceous papules and plaques found over the extensor surfaces of the metacarpophalangeal and interphalangeal joints. These lesions develop scaling that can resolve with dyspigmentation, atrophy and scarring. Gottron’s sign refers to erythematous macules and patches that develop over the extensor surfaces of the elbows and knees. The V sign refers to macular erythema over the anterior neck and upper chest, whereas the shawl sign occurs on the upper back, shoulders and posterior neck. Finally, a heliotrope rash is described as violaceous erythema of the upper eyelids with edema and telangiectasias.4
The rash of carcinoid tumors is different in several ways. First, carcinoid tumors secrete biologically active substances, such as serotonin (5-HT), substance P, histamine, catecholamines and prostaglandins, that escape inactivation by hepatocytes and induce flushing. Midgut tumors produce rashes that are generally rapid, cyanotic and last for less than a minute. These are associated with a mild burning sensation. Foregut tumors produce wheals with pruritus that are reddish-brown and occur over the entire body. Location, lack of scale and pattern distinguish the rash of carcinoid from that of dermatomyositis. Looking for the characteristic symptoms associated with carcinoid can also be very helpful.