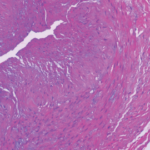
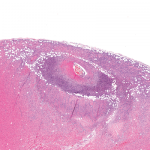
Syphilis is a chronic sexually transmitted disease (STD) caused by the spirochete Treponema pallidum. The clinical manifestations of syphilis are divided into four stages: 1) the primary stage, characterized by painless mucosal or cutaneous chancre at the site of infection that resolves spontaneously; 2) the secondary stage in which a generalized maculopapular rash and condyloma lata are the most characteristic manifestations; 3) the latent stage, which represents a clinically undetectable period; and 4) the tertiary stage, which develops in untreated patients, can affect up to 15–40% of patients and manifests with cardiovascular and neurologic involvement.
Ocular syphilis, previously thought to be uncommon, has drawn renewed interest due to an increase in the number of cases. The incidence has dramatically increased in the U.S. since the early 2000s with re-emergence of syphilis among homosexual males and drug users with concurrent HIV infection.1
The challenge of ocular syphilis is that it can manifest in a number of different ways, with posterior uveitis being the most common.2 Other common manifestations include interstitial keratitis, recurrent anterior uveitis, retinal vasculitis and optic neuropathy.3 Ocular symptoms can occur as early as six weeks after transmission, and it may often be the only presenting feature of systemic syphilis. Patients usually present with complaints of blurry vision and are at risk of permanent blindness if left untreated.
Patients with large vessel vasculitis, such as giant cell arteritis (GCA), can present with a spectrum of vision changes. Sudden monocular visual loss, particularly in an older adult, from arteritic anterior ischemic optic neuropathy (AAION) is a feared complication of GCA because it can lead to complete visual loss.4
Our case highlights some of the similarities between these two conditions.
Case Report
A 76-year-old man with a past medical history of coronary artery disease and hyperlipidemia presented to the ophthalmology clinic with acute blurring of vision in the right eye. He had been noticing a black spot in the center of the visual field of the eye for about four days prior to presentation. He also reported distortion of his vision, as well as an inability to read out of the right eye.
Along with the visual changes, the patient reported a sharp pain in the right temple area that had occurred around the same time. He described having right posterior and occipital scalp sensitivity intermittently for the previous year, although he said the pain in the temple was new.