Discussion
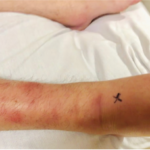
Inflammatory bowel disease-related arthropathy is classified into two types: type 1 is related to disease activity, typically affecting fewer than five large joints. It is usually acute, self-limiting and responds well to inflammatory bowel disease-related treatment in most cases.
Type 2 is more chronic and remains for years; in some cases, it has been associated more with uveitis.2
Because our patient’s symptoms were relatively acute, his arthritis would more likely be classified as type 1; however, because he was on infliximab, we would expect the arthritis to be under control. It’s possible that infliximab was not enough to control his inflammatory bowel disease symptoms, and therefore, he had persistent diarrhea and inflammatory bowel disease arthropathy.
It’s important to consider other possible etiologies of the patient’s arthritis, including reactive arthritis. There are two major types of reactive arthritis, depending on the causative organism. The first type is related to post-enteric infections, classically described with Salmonella, Shigella, Campylobacter and Yersinia. The second type is associated with post-venereal infections, mostly Chlamydia trachomatis.3 Lately, C. difficile infection has been implicated as a less common causative organism.1
C. difficile infection is the most common gastrointestinal infection in patients with inflammatory bowel disease.4 According to recent literature, the prevalence of C. difficile infection has increased in the past decade, and it has been associated with worse prognosis and outcomes.5 In this patient, a diagnosis of C. difficile infection-associated reactive arthritis spared him unnecessary changes in his immunosuppressive treatment plan.
This case was challenging because the patient also had a history of complicated inflammatory bowel disease, raising a suspicion for possible inflammatory bowel disease-related arthritis. However, his condition was controlled, making that diagnosis less likely. Given the patient’s ongoing diarrhea while undergoing aggressive treatment with infliximab, his immunosuppressed state, elevated inflammatory markers, the elevation of his white blood cell counts and the evidence of C. difficile infection in the setting of large joint oligoarthritis in a young adult, reactive arthritis was a more likely diagnosis.6
Conclusion
We described a challenging case of a young man who was referred for consultation of possible newly developed inflammatory bowel disease-related arthritis. On evaluation, he was found to have reactive arthritis secondary to C. difficile infection, which is a rare but well-recognized causative agent for this condition.
This case highlights the importance of keeping an open mind and considering a broad range of possible diagnoses when evaluating rare and complicated conditions, integrating different elements of a patient’s historical information and current workup. Clinicians should maintain a high index of suspicion for rare manifestations of common etiologies.