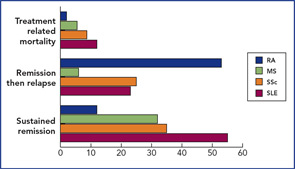
Although anecdotes have a limited place in clinical research, the experience of seeing a young scleroderma patient go from an exhausted and hidebound patient to a near normal individual over three to six months has inspired many of the investigators to push on with the prospective trials to reach the correct conclusion. We owe this to those patients who have put their trust in the program already, not all of whom have done well.
Multipotent MSC for Autoimmune Diseases
Mesenchymal stromal cells (MSCs) are also referred to as mesenchymal stem cells, though their true “stemness” has yet to demonstrated.11 MSCs are capable of differentiating in vitro and in vivo to different MSC lineages, including adipose, bone, cartilage, muscle, and myelosupportive stroma. MSCs may be isolated from bone marrow, skeletal muscle, adipose tissue, synovial membranes, and other connective tissues of human adults, as well as cord blood and placental products, and are defined by using a combination of phenotypic markers and functional properties.
In vitro, MSCs have vast proliferative potential, can clonally regenerate, and can give rise to differentiated progeny. These cells also exhibit anti-proliferative and anti-inflammatory properties in vitro and in vivo, making them candidates for treatment of acute inflammatory autoimmune disease.12 Regardless of whether or not MSCs are true stem cells, clinical benefit from MSCs may not require sustained engraftment of large numbers of cells or differentiation into specific tissues. It is possible that a therapeutic benefit can be obtained by local paracrine production of growth factors and a provision of temporary antiproliferative and immunomodulatory properties.
MSCs enjoy a degree of immune privilege in that allogeneic MSCs may be infused into patients without any preconditioning and seem to survive long enough to exert positive clinical effects without acute toxicity.
The mechanisms underlying the immunosuppressive effect of MSCs remain to be fully clarified, with sometimes-conflicting data probably reflecting the variable definitions and experimental conditions. Certainly, mechanisms may be multiple and involve both cell contact and the production of soluble factors including interleukin (IL)-10, transforming growth factor-beta, hepatocyte growth factor, IL-1 receptor antagonist, and soluble HLA-G.
Animal Models
It may be impossible to try to separate the anti-inflammatory, immunomodulatory, and tissue protective “trophic” effects of MSC. An immunosuppressive effect of MSC in vivo was first suggested in a baboon model, where infusion of ex vivo expanded donor or third-party MSCs delayed the time to rejection of histoincompatible skin grafts. In murine models, MSCs can also down-regulate bleomycin-induced lung inflammation and fibrosis, if given early (but not late) after the induction. A similar effect was observed in a murine hepatic fibrosis model (carbon tetrachloride-induced) using an MSC line. Tissue protective effects were also seen in a rat kidney model of ischemia/reperfusion injury in which syngeneic MSCs were used.