Image Credit: Molodec/shutterstock.com
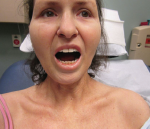
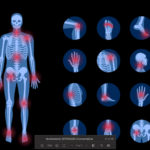
Case report: A 78-year-old Caucasian female presented to our outpatient rheumatology clinic with pain in her bilateral shoulders, hands and knees that began suddenly one month earlier. She admitted to stiffness in her hands lasting several hours, and expressed an inability to extend her fingers. She denied fever, rashes, jaw claudication, headache or visual changes. She also denied having night sweats, unintentional weight loss, shortness of breath or abdominal pain.
Her past medical history was unremarkable, with no prior history of malignancy. She did not take any medication. Her vital signs were stable, and she was afebrile. She had normal breath sounds and a regular heart rate and rhythm. She exhibited no abdominal tenderness.
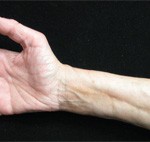
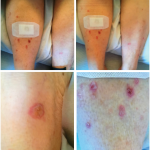
The physical exam was notable for tenderness of both shoulders, with limited range of motion. She had bilateral hand swelling with tenderness to palpation of the palms and proximal and distal interphalangeal joints. She had multiple flexion contractures, with erythema noted extending over the palms and digits (see Figures 1A & 1B). She had no sclerodactyly, nail pitting, Raynaud’s phenomenon or telangiectasias, and no proximal muscle weakness was evident. She had very small effusions in both knees, but the volume was insufficient to aspirate.
Pertinent lab results included a negative rheumatoid factor (RF), negative cyclic citrullinated peptide (CCP) antibodies and a negative result for antinuclear antibodies (ANA). A myositis antibody panel was also negative. Serum creatine kinase level was 36 u/L (normal range 24–173). The erythrocyte sedimentation rate (ESR) was 23 mm/hr (normal range 0–40). The C-reactive protein (CRP) was strikingly elevated at 67.1 mg/L (normal range 0.0–4.9). The complete blood count, electrolytes and hepatic function panel were normal. A chest X-ray was normal, and X-rays of both hands showed mild osteoarthritic changes with joint space narrowing to the proximal interphalangeal and distal interphalangeal (DIP) joints on digits 2–5 bilaterally. Bilateral knee X-rays were normal.
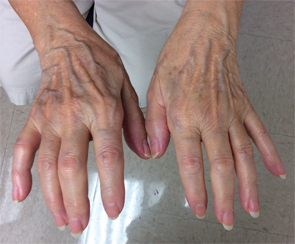
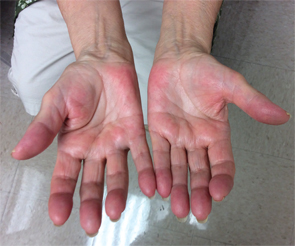
Figure 1A (left) & Figure 1B: These images show the patient’s hands on initial presentation to the rheumatologist, with visible flexion contractures of all digits and swelling, erythema and pain on palpation.

Dr. Kesselman
A diagnosis of palmar fasciitis and polyarthritis syndrome (PFPAS) was rendered. The patient was started on 20 mg prednisone daily with a slow taper planned, and she was advised to follow up with her primary care physician for cancer screening. She had a DEXA scan performed, which showed a normal bone density, with a lumbar spine T score of –0.7, and a hip T score of –0.9. She refused treatment for prevention of glucocorticoid-induced osteoporosis, but agreed to take daily calcium and Vitamin D.