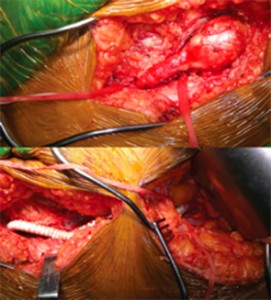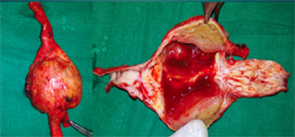
Figure 4. Surgical specimen showing aneurismal dilation and thrombus.
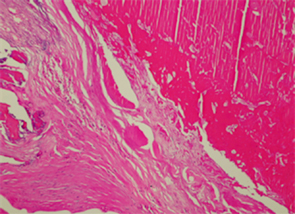
Figure 5. Histopathology image showing intraluminal thrombus with disorganized elastic lamina of the media and scanty inflammatory infiltrate.
Surgical treatment should be done only after adequately treating with immunosuppressive medications (see Table 2). Surgical indications include severe uncontrolled renovascular hypertension, coarctation of the aorta, severe cerebral ischemia, severe aortic regurgitation and progressive aneurismal enlargement or dissection. Surgical bypass procedures have good long-term survival rates, with restenosis rates being less than 30%.3,4 The surgical procedures can be done either by open procedures or through endovascular approach with the use of either autologous or synthetic grafts.
Back to the Case
Our patient had aneurysms at more than one site. There was rapid worsening of the aortic aneurysm leading to rupture. He was fortunate to have survived that and improved after an extensive emergency surgery. Although the femoral artery aneurysm was asymptomatic, because it was reasonably large and had the potential to rupture, elective surgery was done after a six-month period of escalated immunosuppression.