Introduction: Major advances in the past two decades have enhanced our understanding of the complex interactions between the immune system and cancer cells and their environment. Genetic and epigenetic alterations in tumor cells result in the expression of diverse antigens that can elicit an immune response, primarily mediated by T cells. Immune responses are regulated by stimulatory, costimulatory and inhibitory (checkpoint) signals. Inhibitory signals play an important role in self-tolerance under normal conditions. In the presence of tumor cells, immune checkpoint pathways can be disrupted, resulting in tumoral immune resistance.
In the past few decades, several approaches have been proposed to enhance host antitumor responses. Among the most salient strategies is the use of monoclonal antibodies against regulatory immune checkpoint molecules that inhibit T cell activation. These agents up-regulate immune function by blocking checkpoint inhibition, resulting in durable tumor responses in patients with metastatic disease that are not seen with traditional chemotherapy.
Nonetheless, despite its impressive therapeutic benefits, checkpoint blockade can induce profound inflammatory and immune-related adverse events (AEs), which can be severe and limit use of checkpoint inhibition.
This review article discusses tumor immunity; immune checkpoint inhibitors for the treatment of cancer, including the four checkpoint inhibitors currently FDA approved: ipilimumab (a CTLA-4 inhibitor), pembrolizumab and nivolumab (anti–programmed cell death 1 [anti–PD-1]) and atezolizumab (anti–PD-L1); treatment of immune-related AEs with checkpoint inhibitors; and use of checkpoint inhibitors in patients with cancer and preexisting autoimmune disease.
Adverse Events
Some AEs occur more frequently with a given agent. In general, anti–PD-1 agents appear to be better tolerated; they can trigger AEs similar to those associated with ipilimumab, including dermatitis and hepatotoxicity, with some variations. The toxicity of newer anti–PD-L1 agents is not as well described. Combination therapy, compared with monotherapy, increases the frequency of AEs.
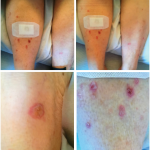
Skin manifestations are the most common AEs seen with all checkpoint inhibitors. Diarrhea occurs in up to 30% of patients receiving ipilimumab and less frequently in patients receiving anti–PD-1 therapy. Several endocrinopathies have been reported in patients receiving checkpoint blockade. Thyroiditis is the most commonly reported AE. Elevated levels of hepatic enzymes can be observed in about 5% of patients, more frequently in those receiving combination therapy. Pneumonitis has been observed more frequently in patients treated with nivolumab. Arthralgia has been observed in about 15% of patients receiving checkpoint blockade. However, the incidence of inflammatory arthritis has not been systematically reported.
The clinical treatment of patients receiving checkpoint blockade and developing an AE requires a multidisciplinary patient-centered approach. One study proposed a useful clinical framework for the management of AEs, including prevention, anticipation, detection, treatment and monitoring. Risk factors for autoimmunity need to be carefully evaluated before starting treatment to ensure personalized monitoring and prompt recognition of AEs.