 Mast cells play an important role in the pathogenesis of degenerative musculoskeletal diseases and chronic pain conditions. Recent work has revealed that mast cells perform a critical function in the pathophysiology of osteoarthritis. Now, scientists have turned their attention to the role of mast cells in low back pain.
Mast cells play an important role in the pathogenesis of degenerative musculoskeletal diseases and chronic pain conditions. Recent work has revealed that mast cells perform a critical function in the pathophysiology of osteoarthritis. Now, scientists have turned their attention to the role of mast cells in low back pain.
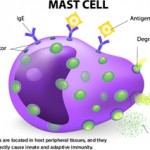
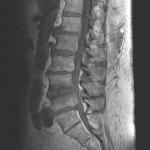
Researchers looked specifically at the intervertebral disc, which contains three integrated structures: the inner gelatinous nucleus pulposus (NP), the outer lamellar annulus fibrosus (AF) and the cartilaginous endplates (EP) that connect the invertebral discs to the vertebral bodies. A healthy intervertebral disc is considered immune privileged, and the disc—in particular the AF—acts as a physical and biochemical barrier to inflammation and immune cell infiltration. However, during aging, degeneration and/or injury, mast cells can enter the intervertebral disc. Although scientists have documented the presence of mast cells in painful discs, the role of mast cells in low back pain and intervertebral disc degeneration is still not well understood.
Recent research published online on Oct. 2 in Scientific Reports revealed that mast cells can infiltrate intervertebral disc cells and play a key role in their degeneration.1 The investigators designed their study to better understand the presence and role of mast cells within the intervertebral disc. Matthew G. Wiet, a medical student at Ohio State University, Columbus, and colleagues found that not only can mast cells affect the function of intervertebral disc cells, but intervertebral disc cells can also affect the function of mast cells.
“To our knowledge, this is the first study to explicitly explore the presence and function of mast cells in the intervertebral disc,” write the authors in the conclusion of their paper. “Here we demonstrated that mast cells are present in the painful [intervertebral disc] and that they likely play a key role in degeneration of the [disc]. We provide evidence that mast cells are able to 1) stimulate an inflammatory and catabolic phenotype in [intervertebral disc] cells specifically NP and EP cells, and vice versa, and 2) that healthy annulus fibrosus cells can inhibit activation of mast cells and a pro-angiogenic phenotype in these cells.”
The investigators used immunohistochemistry and 3D in vitro cell culture methods to characterize mast cell–intervertebral disc cell interactions. They began their work by using immunohistochemistry staining to investigate the presence of mast cell-specific markers within the human intervertebral disc. They examined painful intervertebral discs that had been surgically removed from patients and compared them with cadaveric intervertebral discs. Study limitation: The researchers assumed the cadaveric discs came from individuals who had died without back pain because the discs were intact upon the patient’s death. The researchers did not indicate that any efforts were made to determine whether the individuals had actually been living with pain prior to their deaths. This flaw appears to be reflected in the data: 19.3% of cadaveric samples had mast cells.