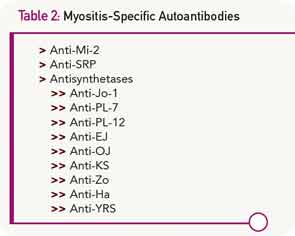
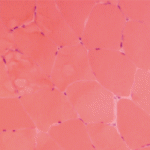
The Differential Diagnosis Is Huge
Another challenge in diagnosing idiopathic inflammatory myopathies involves differentiating them from many other conditions, considered to be myositis mimics, which can also fulfill Bohan and Peter’s criteria (see Table 1). Bohan and Peter recognized the relative nonspecific nature of their criteria, stating, “There are certain findings, herein called exclusions, whose presence should make one very cautious about rendering a diagnosis of polymyositis.”2
The first group of myositis mimics are muscular dystrophies. These are inherited disorders characterized by progressive muscle weakness that advances to muscle wasting. Becker, limb-girdle, and facioscapular dystrophies may present in late adolescence or adulthood with proximal muscle weakness and elevated muscle enzymes. Although the classic histologic picture in these diseases includes muscle-fiber size variation with necrosis and eventually replacement of muscle by fat and fibrous tissue, inflammatory cells may also be observed in early stages. The situation may be further complicated by the observation that some patients with muscular dystrophy note a temporary improvement with corticosteroid therapy.
Selected infections can cause a chronic myopathy. This is particularly true for immunocompromised individuals in whom toxoplasmosis infection can result in the development of an inflammatory myopathy. Some patients infected with HIV develop a slowly progressive proximal myopathy with elevated CPK levels. Muscle biopsy demonstrates endomysial, perimysial, or perivascular mononuclear cell infiltrates and muscle fiber necrosis.
Many drugs can induce a myopathy. Corticosteroids and HMG-CoA reductase inhibitors (statins) are among the most common. Corticosteroid use can result in the development of painless proximal muscle weakness, especially involving the pelvic girdle muscles and neck flexors. In patients being treated for diseases other than myositis, the serum CPK is normal and magnetic resonance imaging of the muscles is unremarkable. EMG may show low-amplitude motor unit potentials, and muscle biopsy classically demonstrates type 2 fiber atrophy. The clinical picture may be confounding when a myositis patient treated with corticosteroids initially improves to a degree and then begins to regress. Is the myositis flaring, or is there a superimposed corticosteroid myopathy? Generally, the latter condition occurs in patients who have been treated with corticosteroids for at least four weeks or, in most cases, for much longer. It is more likely to occur in patients treated with higher doses of corticosteroids, especially the fluorinated preparations (triamcinolone, dexamethasone, or betamethasone). One strategy to diagnose steroid myopathy is to rapidly taper the dose and see if there is clinical improvement or worsening.