Brian Goodman/shutterstock.com
CHICAGO—Despite the complicated politics surrounding medical marijuana, cannabis has a wide variety of medical benefits and potential benefits, but the risks need to be understood, said Daniel Clauw, MD, director of the Chronic Pain and Fatigue Research Center at the University of Michigan, in a session at the ACR’s 2016 State-of-the-Art Clinical Symposium.
Effects
It’s important to understand the body’s endocannabinoid system to understand how the drugs work, he said. The system is a set of receptors and their natural ligands, plus enzymes that regulate them. There are two main receptor types: CB1, which mainly affects the central nervous system and the brain, and CB2, which is found in the periphery and affects the immune system and nerve cells.
The known functions of endocannabinoids are disruption of short-term memory, which can have a positive medical impact in the case of something like post-traumatic stress disorder, neurogenesis, neuroprotection, appetite increase, analgesia, immune function and stress.
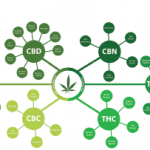
Of the 80 cannabinoids found in cannabis plants, the two most important are tetrahydrocannabinol (THC) and cannabidiol (CBD). THC has mostly CB1-type effects on the central nervous system. Cannabidiol has no psychoactive effects, and it’s not clear where it binds in the body, but it appears to protect against the psychoactive effects of THC.
“We don’t know what the optimal ratio of THC to CBD is,” Dr. Clauw said. “We know it’s likely good to have some CBD.”
‘Even if we end up replacing one problem for another, [marijuana] is a safer addiction, if you will, than the opioid addiction.’ —Daniel Clauw, MD
The cannabis-based Marinol is FDA approved for nausea after chemotherapy and AIDS-induced anorexia. Cannabinoids also might have anti-spasmodic effects and neuroprotective effects. In one study, researchers examined marijuana drug-test results of people in a neurologic intensive care unit for head trauma. Those whose test for THC was positive did much better with the injuries than those who’d had a negative test. As Dr. Clauw noted, it wasn’t a randomized trial, but “the differences were pretty profound.”1
Canabinoids’ anti-inflammatory effects are being studied now at The Feinstein Institute in a trial of ajulemic acid, a cannabinoid with low potential for psychoactive effects because it has far greater selectivity for CB2 than CB1 and doesn’t get into the CNS very well. It is now being studied in lupus.
Pain Relief
Both CB1 and CB2 agonists, as well as a mixture, have been found to be effective in animal models of pain, Dr. Clauw said. They work in basically the same way opioids work—not by actually doing away with pain, but by dissociating people from the unpleasantness of pain. But much of the mechanism of action isn’t known because of the lack of NIH-funded research on the subject.

Dr. Clauw