Introduction & Objectives
Immunoglobulin G4-related disease (IgG4-RD) can cause fibroinflammatory lesions in nearly any organ and may be confused with malignancy, infection or other immune-mediated conditions, such as Sjögren’s syndrome or vasculitis, associated with anti-neutrophil cytoplasmic antibodies (ANCAs). Rheumatologists, internists, gastroenterologists, nephrologists, pulmonologists, neurologists, radiologists, pathologists and other practitioners are often involved in the evaluation of patients with this condition. IgG4-RD can lead to organ dysfunction, organ failure and death. Its epidemiology remains poorly described because of its relatively recent recognition (2003) as a discrete condition, yet the disease is now seen by generalists and specialists all across the world.
Although clinical, serologic, radiologic and pathologic features all contribute to the classification of IgG4-RD, none of these approaches alone provides definitive evidence for the accurate classification of patients. The proper categorization of patients for both research studies and clinical purposes relies upon integration of data from all four evidence domains. This study was undertaken to develop and validate an international set of classification criteria for IgG4-RD.
Methods
An international multispecialty group of 86 physicians was assembled by the ACR and the European League Against Rheumatism (EULAR). Investigators used consensus exercises, existing literature, derivation and validation cohorts of 1,879 subjects (1,086 cases, 793 mimickers), and multicriterion decision analysis to identify, weight and test potential classification criteria. Two independent validation cohorts were included.
Results
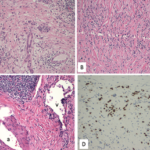
A three-step classification process was developed: First, it must be demonstrated that a potential IgG4-RD case has involvement of at least one of 11 possible organs (i.e., pancreas, salivary glands, bile ducts, orbits, lacrimal glands, kidneys, lungs, aorta, retroperitoneum, pachymeninges or thyroid gland [Riedel’s thyroiditis]) in a manner consistent with IgG4-RD. Second, exclusion criteria consisting of a total of 32 clinical, serologic, radiologic and pathologic items must be applied; the presence of any of these criteria eliminates the patient from IgG4-RD classification. Third, eight weighted inclusion criteria domains, addressing clinical findings, serologic results, radiology assessment, and pathology interpretations, are applied.
In the first validation cohort, a threshold of 20 points had a specificity of 99.2% (95% confidence interval [95% CI] 97.2–99.8%) and a sensitivity of 85.5% (95% CI 81.9–88.5%). In the second, the specificity was 97.8% (95% CI 93.7–99.2%), and the sensitivity was 82.0% (95% CI 77.0–86.1%). The criteria were shown to have robust test characteristics over a wide range of thresholds.
Conclusion
ACR/EULAR classification criteria for IgG4-RD have been developed and validated in a large cohort of patients. These criteria demonstrate excellent test performance and should contribute substantially to future clinical, epidemiologic and basic science investigations.
Reminder: Classification criteria are not diagnostic criteria. Thus, some patients with clinical diagnoses of IgG4-RD will not fulfill these classification criteria. If a healthcare provider feels a patient has IgG4-RD, then that patient should be treated for IgG4-RD.