Autoinflammatory diseases should be suspected when a patient presents with recurrent episodes of fevers that recur over months or years in the absence of an associated viral or bacterial infection, and when autoimmune disease and malignancies have been excluded. The new guidelines address the following recurrent fevers, defined in terms of their mutation and their clinical manifestations:
- Familial Mediterranean fever, defined by presence of the MEFV gene, which provides instructions for making a protein called pyrin, and presenting at least one of the following: arthritis, chest pain or abdominal pain;
- Tumor necrosis factor (TNF) receptor-associated periodic fever syndrome, defined by confirmation of the TNF genotype and presence of myalgia, migratory rash, periorbital edema and/or familial connections;
- Mevalonate kinase deficiency, defined by mutations in the MK gene and presence of gastrointestinal symptoms, cervical lymphadenitis or aphthous stomatitis; and
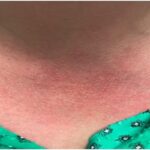
- Cryopyrin-associated periodic syndrome, defined by a mutation of NLRP3 and presence of urticarial rash, red eye or neurosensorial hearing loss.
The new analysis also incorporates undefined recurrent fevers and a related group of more common non-hereditary, periodic fevers, aphthosis, pharyngitis and adenitis, which tend to be more common in children.
A Complicated Process to Reach Consensus
The development of the new guidelines was spearheaded by lead author Marco Gattorno, MD, Istituto Giannina Gaslini, Genoa, Italy, and by the Paediatric Rheumatology International Trials Organization (PRINTO), which links European centers that are following patients diagnosed with, or suspected of having, these disorders. PRINTO says fragmentation of treatment for these cases exists across different treatment centers and countries due to the lack of classification criteria.
A large group of European and North American researchers were asked to participate in a lengthy, multi-step process that included periodic online communication, an in-person meeting in March 2017 and a lot of heated discussions, Dr. Hoffman says. The process started with selection of clinical, laboratory and genetic candidate variables and cross-sectional validation by an international panel of experienced clinicians using the statistical evaluation of real patients for which researchers had both genetic information and good clinical phenotypes.
Clinical information on an initial group of 360 patients from PRINTO’s Eurofever Registry was presented to a panel of 25 clinician researchers and eight geneticists, who were asked to propose their best educated guesses on classification. Disease consensus was achieved for inclusion of 281 (78%) of these 360 initial patients.
“We were then given the genetic information and asked if that would change our minds about the initial classification. They brought us all together in beautiful Genoa, Italy, to talk about our experience with these diseases,” Dr. Hoffman says. “The process taught us all about our misconceptions.”