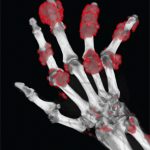
We read the case report by Dr. Diana Girnita and colleagues (“Severe Refractory Gout: What options are left when pegloticase fails?” The Rheumatologist, August 2016) with interest. A case is reported of a subject with 20 years of chronic refractory gout who failed to respond to pegloticase therapy, and the potential roles of anti-drug antibodies or genetics are discussed. We would like to point out another possible—and we believe more likely—explanation for the findings in this case.
As opposed to the claim of Dr. Girnita that “all patients given pegloticase initially had significant decreases in their PUA,” a review of the database from the randomized clinical trials of pegloticase in chronic refractory gout indicates that two of the 85 subjects (2.4%) receiving 8 mg of pegloticase every two weeks failed to reduce their uric acid levels significantly two weeks after initial treatment. Following subsequent infusions, these subjects also had no significant lowering of their uric acid levels and were categorized as nonresponders. These results indicate that a small fraction of subjects fail to respond to pegloticase. Dr. Girnita suggests this might be related to the development of anti-drug antibodies as we previously reported1 or the possibility of a role for genetic alterations of uric acid transporters. However, a more detailed analysis of these two subjects suggests a different interpretation.
Although neither of these subjects exhibited significant urate lowering two weeks post infusion, each manifest very significant lowering of plasma uric acid 24 hours post infusion (1.03 mg/dL and 1.95 mg/dL, respectively). Moreover, each exhibited a quite low peak pegloticase level after the initial infusion (0.6 and 0.9 ug/mL), whereas the mean peak level in pegloticase treated subjects was 1.4+/-0.1 ug/mL.1 Because the mean terminal half-life of pegloticase is 214 hours (8.9 days), it’s not surprising that these subjects would have very little pegloticase present two weeks after the infusion (0 ug/mL, 0 ug/mL, respectively) and, therefore, minimal urate lowering activity. The explanation of the altered pharmacokinetics in these two subjects is not certain, but weight and related expanded volume of distribution could have contributed because both subjects were quite large, weighing 137 kg (BMI 38.9) and 109 kg (BMI 37.7), respectively. We were not told of the weight or BMI of the subject in the Girnita report. It is unlikely that pre-formed anti-drug antibodies played a role because they were not detected in either subject before treatment. It is possible, however, that the early development of anti-drug antibodies played a role in one subject because anti-pegloticase antibodies at a titer of 1:2430 were detected in this subject two weeks after the first infusion.
In summary, it is likely that the pharmacokinetics of pegloticase rather than the genetic profile of urate transporters played an important determinant in the success of pegloticase therapy reported in the case reported by Dr. Girnita. Because the mechanism of pegloticase involves metabolizing uric acid to soluble products largely in the circulation regardless of the reason it is elevated, it is difficult to imagine how the mechanism of urate elevation would be a determinant of its effectiveness. However, the capacity to degrade urate is directly related to its presence and concentration in the circulation, and factors that affect those parameters, including anti-drug antibodies of sufficient titer (>1:2430) and characteristics of the subject, such as body mass and volume of distribution, will certainly have an effect.
In rare subjects, such as the one described by Dr. Girnita, who fail to lower their urate two weeks after the first dose, more frequent urate monitoring might be considered, as well as more frequent dosing as is currently being tested in the Tolerization Reduces Intolerance to Pegloticase and Prolongs the Urate Lowering Effect (TRIPLE) protocol (NCT 02598596).
Sincerely,
Peter E. Lipsky, MD
Anthony Yeo, MBBS, PhD, MPH
Reference
- Lipsky PE, Calabrese LH, Kavanaugh A, et al. Pegloticase immunogenicity: The relationship between efficacy and antibody development in patients treated for refractory chronic gout. Arthritis Res Therapy. 2014 Mar 4;16(2):R60.
The authors reply: We appreciate the interest shown by Dr. Lipsky and Dr. Yeo in our case and are grateful for their insight into our patient’s case.
Our patient had a BMI of 37, and it appears that he might be consistent with the two individual failures reported by Lipsky et al. Pegloticase levels were not measured in our patient post infusion and uric acid levels were not checked 24 hours post infusion. Thus, based on the current information, we cannot confirm whether altered pharmacokinetics due to obesity played a role in our patient’s suboptimal response. So this remains a speculative, yet quite likely explanation.
We eagerly await the completion and results from the TRIPLE study (NCT 02598596) to guide us with regard to the dosing intervals in similar patients. If the relationship between BMI and drug efficacy is found to be true, this will significantly impact the dosing regimen, especially with the current high prevalence of obesity.
—Diana M. Girnita, MD, PhD, Cody Lee, MD, & Christine Chhakchhuak, MD