The Japanese have described IgG4-related disease as a “crow flying in the night.”
LiuSol/shutterstock.com
CHICAGO—Researchers have come to know a great deal about IgG4-related disease in a short amount of time, leading to effective treatments with the prospect for more, an expert said at the 2016 State-of-the-Art Clinical Symposium.
“One of the most exciting things for me is how quickly we’ve been able to move in understanding this disease,” said John Stone, MD, MPH, professor of medicine at Harvard Medical School, Boston. He recalled a patient from several years before with swollen glands. At the time, Dr. Stone had no idea what she had.
But today, there is a fairly well-developed pathogenic picture of what is happening in the disease, said Dr. Stone, who gained clues into what is now known to be a multi-organ disorder by reviewing isolated case studies in the literature dating as far back as 1899.1
Distinctive Features
One Japanese study, from 2001 in the New England Journal of Medicine, described the way pancreatitis in patients with elevated IgG4 serum levels was different from pancreatitis associated with other hepatobiliary diseases: enlarged, swollen and sausage shaped. These IgG4 levels were affecting many organs, but it wasn’t recognized as doing so. Undetected for what it was, the Japanese described it as a “crow flying in the night.”2
“Over the last dozen years, this crow has flown into full light, and we recognize that this disease really can involve every single organ in the body,” Dr. Stone said.
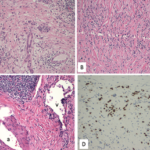
The three hallmarks of the disease that are seen on pathology are a swirling, pink fibrosis or “storiform fibrosis”; a preponderance of plasma cells in that infiltrate staining positive for IgG4; and obliterative phlebitis or lymphoplasmacytic infiltrate moving right through veins and other structures.
This pathology is the same regardless of the organ, whether it’s the kidneys, lungs or even the meninges.
Mass lesions and atopic features—including asthma, allergic rhinitis and nasal polyps—are commonly seen in the disease. One of the more distinctive features, seen in about 12% of patients, is a kind of paravertebral mass that isn’t seen in any other kind of disorder.
Treatment
B cell depletion with rituximab has been found to bring about dramatic improvement in physical symptoms, such as gland size, and in serum IgG4 levels, by depleting the supply of CD20-positive B cells, important players in the disease that are responsible for producing IgG4-producing plasmablasts.3 He discussed rituximab’s effects in one patient, for example, who had a sudden drop in B cells and plasmablasts after treatment, after which the B cell level rebounded, but the plasmablast level remained low, keeping the patient in remission.