A 47-year-old Caucasian woman presented to the rheumatology clinic with a one-year history of pain and swelling involving the wrists, hands, ankles and feet that progressively worsened. Her symptoms included generalized fatigue, morning stiffness in the hands and lower back lasting more than an hour, Raynaud’s phenomena (triphasic), photosensitivity, tightening of the skin of the hands and feet, heartburn, chest wall tenderness, exertional dyspnea, sicca symptoms and an unintentional weight loss of 30 lbs. over the prior six months.
She had previously been evaluated by another rheumatologist for a four-year history of lower back pain associated with stiffness, which was relieved by non-steroidal anti-inflammatory medications (NSAIDs) and activity. Imaging of the sacroiliac joints revealed bilateral sacroiliitis, and she was diagnosed with ankylosing spondylitis.
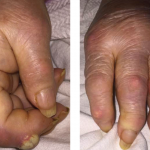
One year before, she was also given the diagnosis of scleroderma, due to symmetrical skin thickening distal to the MCPs, synovitis of her MCP and PIP joints, the presence of Raynaud’s phenomenon and a history of esophageal reflux symptoms. She was treated with prednisone 20 mg daily and hydroxychloroquine 200 mg twice daily with minimal improvement in her symptoms.
Medical History
Her medical history was remarkable for hypertension, hypothyroidism and right carpal tunnel release. She was up to date on risk- and age-appropriate malignancy screenings, including mammogram, pap smears and vaccinations.
Social & Family History
The patient was born and raised in Michigan and is happily married with two healthy children. She is employed and is a nonsmoker. She denies chronic alcoholism or illicit drug use. There is no family history of an autoimmune disease.
Physical Examination
At the time of presentation, she was in no acute distress, with a blood pressure of 156/97 mmHg, pulse of 82 beats/min, oxygen saturation of 97% on room air, afebrile and a BMI of 22.9 kg/m2.
Her physical exam was remarkable for synovitis involving the metacarpophalangeal joints bilaterally, sclerodactyly distal to the MCPs bilaterally, dusky bluish cold extremities with no ulcerations, chest wall tenderness at the costovertebral junction and over the manubrium, diffuse bilateral inspiratory fine crackles, tenderness in the gluteal region bilaterally and a positive Patrick’s test. Nail fold capillaroscopy revealed altered capillary distribution. No facial telangiectasias were noted.
Laboratory Evaluation
Laboratory workup revealed a normocytic anemia with a hemoglobin of 10.9, MCV 90, ESR 65, CRP 2.6, positive IF-ANA (1:1280 speckled), RNP titer of 159, SSA 135, SSB 74, positive anti-centromere antibodies and a positive HLA-B27. Chemistry panel, urine analysis, RF, CCP, anti-Smith antibodies, C3, C4, anti-dsDNA, anti-phospholipid antibodies and ANCA titers were within normal ranges.