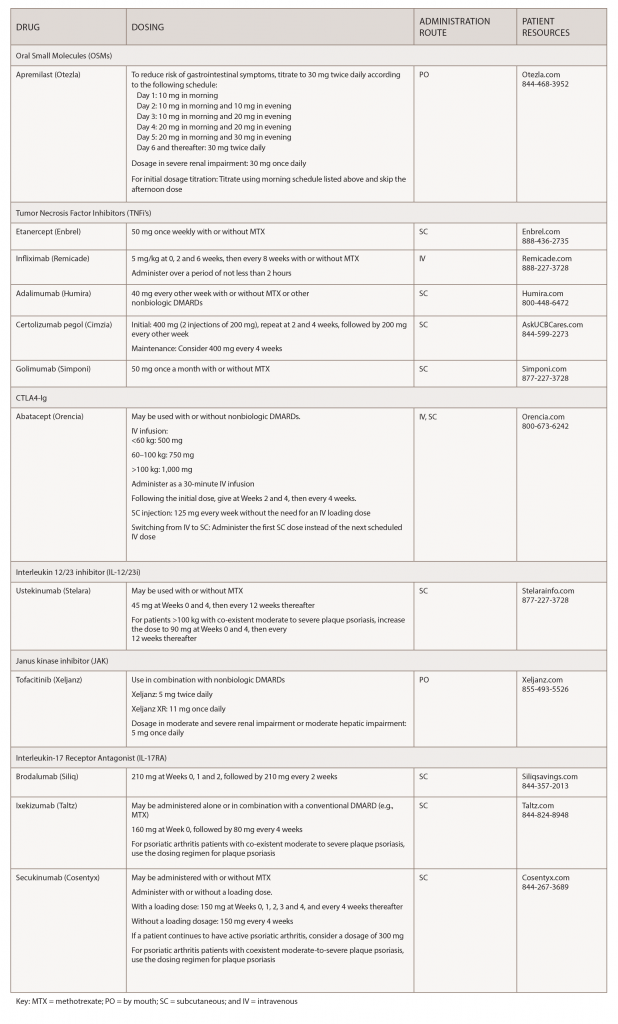
Over the past few years, biosimilars and other new drugs have been introduced to treat rheumatic illnesses. Some of the conditions we treat have numerous drug options, others have few or only off-label options. This series, Rheumatology Drugs at a Glance, provides streamlined information on the administration of biologic, biosimilar and other medications used to treat patients with rheumatic disease. In Part 1 of this series, we discuss the 19 available options to treat psoriatic arthritis (see Table 1).
Psoriatic arthritis (PsA) is a chronic inflammatory musculoskeletal disease that remains undertreated in patients. Clinicians and patients can now choose from a wide variety of pharmacological therapies to control the signs and symptoms, and improve physical function and quality of life by slowing the disease progression and saving joints and other tissues from permanent damage. Standard and biologic disease-modifying anti-rheumatic drugs (DMARDs) may reduce symptoms and attempt to slow PsA disease progression, while non-steroidal anti-inflammatory drugs (NSAIDs) and steroids can be used for pain management and to reduce joint swelling.1
Early diagnosis of PsA and prompt initiation of therapy are important to improve long-term outcomes. Even a six-month delay from symptom onset to the first visit with a rheumatologist contributes to the development of peripheral joint erosions and can worsen long-term physical function.2
Adherence to treatment is crucial for patients to achieve and maintain remission. But patient dissatisfaction with treatment options is apparent when they don’t see a physician, initiate or continue therapies. Concerns with long-term safety, adverse events, administration challenges and cost abound.3 Additionally, patients may feel better after treatment and decide to discontinue their medications. However, patients who stop their medications report their disease returns within three to six months. Unfortunately, a patient’s chance of achieving drug-free remission is low.4
It is important to advise patients that remission does not equal cure. Once patients stop their medications, the symptoms that return may be worse than before.
An integral part of patient care includes the healthcare provider incorporating patient education into their care and understanding PsA from the patient’s perspective. Patient education includes the provision of educational activities related to the disease, treatment and the consequences of non-adherence.5 A discussion of long-term outcomes is often a highly effective way to encourage adherence. A discussion of potential side effects can help prevent a patient from discontinuing treatment prematurely. Advise patients of the need to stay on treatment to avoid recurrences or flares. It is also important physicians review the signs and symptoms of infections with patients and advise patients to let the provider know if they are experiencing any new infections. Most of the biologic treatments require testing for some infections or pre-vaccination to prevent infections once on treatment.
Treatments for PsA can be expensive, and healthcare providers can help make treatment costs more manageable for patients. A number of financial assistance resources are available to patients, and patients can contact the manufacturer of a medication to request co-pay assistance. Your staff can also explore patient assistance programs for those who do not have insurance.6
Depending on a patient’s healthcare coverage and the medication(s) they use, a specialty pharmacy may dispense the medications. Most specialty pharmacies have clinical pharmacists available who can help patients deal with insurance issues, drug monitoring for adverse effects and effectiveness, and answer medication- or disease-related questions.
For additional information, the ACR and the National Psoriasis Foundation (NPF) have published their first joint guideline for treating psoriatic arthritis. It can be found here.1