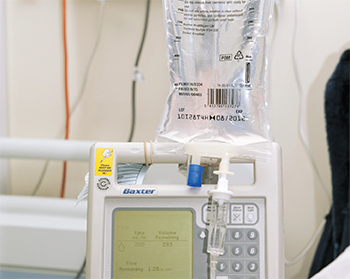
An Intravenous infusion (IV drip) of rituximab is being performed in a hospital setting.
Dr P. Marazzi/Science Source
Rheumatologists prescribe rituximab for induction and maintenance treatment for anti-neutrophil cytoplasm antibody (ANCA) associated vasculitides (AAV). Maintenance treatment typically employs fixed-schedule dosing, but in the recent maintenance of remission using rituximab in systemic ANCA-associated vasculitis II (MAINRITSAN2) trial, researchers from the French Vasculitis Study Group examined whether individually tailored maintenance dosing might work better.
“The main objectives of the MAINRITSAN2 trial were to determine whether an individually tailored infusion strategy would maintain remission with fewer relapses, fewer infusions and fewer infections,” says Loïc Guillevin, professor in the Department of Internal Medicine at Hôpital Cochin at Université Paris Descartes, France. “The other objective was to determine whether a reinfusion strategy based on ANCA and circulating CD19+ B cells would accurately predict relapses.”
The Study Details
The study included patients diagnosed with initial-onset or relapsing granulomatosis with polyangiitis (GPA) or microscopic polyangiitis (MPA) from November 2012–November 2013 who were in complete remission following induction. Of those 162 patients, 117 (72.2%) were diagnosed with GPA, and 45 (27.8%) were diagnosed with MPA.
Patients in this open-label, multicenter trial were randomized to either tailored (n=81) or control (n=81) groups. Controls received a fixed dose of rituximab infusion at Days 0 and 14 following randomization, then at six, 12 and 18 months after the first doses. The tailored patients received the same dose at randomization with reinfusion only when the CD19+ lymphocytes or ANCA reappeared, or ANCA titer rose markedly based on trimestrial testing.

Prof. Guillevin
The patients received intravenous methylprednisolone (100 mg), dexchlorpheniramine (5 mg) and acetaminophen (1,000 mg) before all rituximab infusions. Most were taking low-dose prednisone at randomization, which could be tapered and stopped or maintained at 5 mg/day at the discretion of the site investigator.
Statistical analysis was performed on an intention-to-treat basis. Study visits occurred at enrollment and then every three months until the endpoint, 28 months following randomization. At each visit, a Birmingham Vasculitis Activity Score (BVAS) was calculated. Patients were asked to record their study medication(s) in a weekly diary. ANCA testing and CD19+ B cell counts for a given patient were always determined in the same laboratory.
The primary endpoint was the number of relapses (defined as new, reappearing symptom[s] or a worsening BVAS) at Month 28, as judged by an independent adjudication committee. The committee was blinded to treatment group.