Tefi / shutterstock.com
Genes may predispose people to have certain microbial signatures in their gut that, in turn, make them susceptible to developing reactive arthritis. This is the main finding of a recent study in which researchers investigated whether perturbations in the intestinal microbiome play a role in susceptibility to reactive arthritis in the face of triggers, such as gastrointestinal (GI) or genitourinary (GU) infection.1
The study, “Gut Microbiota Perturbations in Reactive Arthritis and Postinfectious Spondyloarthritis” by Julia Manasson, MD, rheumatology post-doctoral fellow, Division of Rheumatology, Department of Medicine, NYU Langone Health, New York, and colleagues, is the first to use culture-independent, high-throughput DNA sequencing to examine the gut microbiome in patients with reactive arthritis and postinfectious spondyloarthritis.
“Although reactive arthritis is thought to be triggered by certain GI or GU infections, we often do not know in an individual patient what organisms may be responsible,” says Allen Steere, MD, professor of medicine, Harvard Medical School, director of clinical research, Rheumatology Unit, Massachusetts General Hospital, Boston, who commented on the study for The Rheumatologist.
By using a new, DNA sequencing, discovery-based method to determine the range of organisms present in the patients’ stool samples, the investigators found “a broader range of organisms than was previously known in reactive arthritis,” he says, adding that the results “support the hypothesis that certain organisms in the gut may shape immune responses that are important to reactive arthritis.”
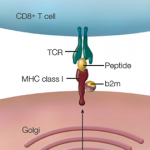
The study also looked at the relationship between host genes and microbiota, and particularly focused on the human leukocyte antigen (HLA) genes. Previous data have shown an association between HLA-B27 and reactive arthritis, although the presence of HLA-B27 does not guarantee the development of disease. Further, HLA-B27 is highly prevalent in Caucasian Northern Europeans, but absent in many other populations in whom reactive arthritis develops.
The current study included patients from Guatemala, an area where there is a low prevalence of the HLA-B27 allele. Only four patients in the study were HLA-B27 positive. The study found that patients who were HLA-A24 positive showed distinct gut microbiota profiles compared with those who were HLA-A24 negative, irrespective of disease status. This was also true in the case of HLA-B35. This finding suggests host genetics contributes to the richness and diversity of gut microbiota.
“Genetics seems to play a role in determining gut microbiota composition,” says lead author Dr. Manasson. “This, in turn, may confer susceptibility to developing disease, [such as] reactive arthritis, when in the presence of other triggers.”