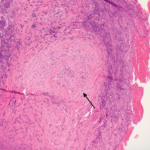
Diagnostic difficulty can lead to a delay in initiation of the proper treatment, and a thorough evaluation of the patient is required to determine the final diagnosis and correct management in a timely manner.
 Harry Subramanian is a medical student at the Yale School of Medicine. He will be pursuing a residency in diagnostic radiology at the Yale-New Haven Hospital.
Harry Subramanian is a medical student at the Yale School of Medicine. He will be pursuing a residency in diagnostic radiology at the Yale-New Haven Hospital.
 Ravi B. Sutaria, MD, is a graduating fellow of Rheumatology at the Yale School of Medicine. Prior to joining Yale he was a clinical instructor of medicine at Jacobi Medical Center at North Central Bronx Hospital in New York during his time as a hospitalist. He is pursuing research establishing the efficacy of DMARDs in the treatment of chronic rheumatism as result of emerging viral infections, such as chikungunya. He is also interested in interventional/diagnostic musculoskeletal ultrasound, particularly in patients with autoimmune and inflammatory disorders.
Ravi B. Sutaria, MD, is a graduating fellow of Rheumatology at the Yale School of Medicine. Prior to joining Yale he was a clinical instructor of medicine at Jacobi Medical Center at North Central Bronx Hospital in New York during his time as a hospitalist. He is pursuing research establishing the efficacy of DMARDs in the treatment of chronic rheumatism as result of emerging viral infections, such as chikungunya. He is also interested in interventional/diagnostic musculoskeletal ultrasound, particularly in patients with autoimmune and inflammatory disorders.
 Fotios Koumpouras, MD, is assistant professor of medicine and director of the Yale Lupus Program. He is an active member of the ACR, the Arthritis Foundation and the Lupus Foundation. In addition to SLE, Dr. Koumpouras has an interest in lupus biomarkers, pregnancy in rheumatic disease, psoriatic arthritis, diagnostic and treatment dilemmas, adolescent arthritis, lupus and the heart, gout and the gender gap of autoimmune disorders.
Fotios Koumpouras, MD, is assistant professor of medicine and director of the Yale Lupus Program. He is an active member of the ACR, the Arthritis Foundation and the Lupus Foundation. In addition to SLE, Dr. Koumpouras has an interest in lupus biomarkers, pregnancy in rheumatic disease, psoriatic arthritis, diagnostic and treatment dilemmas, adolescent arthritis, lupus and the heart, gout and the gender gap of autoimmune disorders.
Disclosures
None of the authors reports any relevant disclosures for this project, but Dr. Koumpouras reports he has previously received grant funding from NIH, NIAMS and Yale University and conducted clinical trials with Merck, Xencor, GSK, Aurinia Pharmaceuticals, UCB and the Lupus Clinical Investigators Network.
References
- Jennette JC, Falk RJ, Bacon PA, et al. 2012 revised International Chapel Hill Consensus Conference Nomenclature of Vasculitides. Arthritis Rheum. 2013 Jan;65(1):1–11.
- Lutalo PM, D’Cruz DP. Diagnosis and classification of granulomatosis with polyangiitis (aka Wegener’s granulomatosis). J Autoimmun. 2014;48–49:94–98.
- Comarmond C, Cacoub P. Granulomatosis with polyangiitis (Wegener): Clinical aspects and treatment. Autoimmun Rev. 2014 Nov;13(11):1121–1125.
- Grant SC, Levy RD, Venning MC, et al. Wegener’s granulomatosis and the heart. Br Heart J. 1994 Jan;71(1):82–86.
- Mahr A, Batteux F, Tubiana S, et al. Brief report: Prevalence of antineutrophil cytoplasmic antibodies in infective endocarditis. Arthritis Rheumatol. 2014 Jun;66(6):1672–1677.
- Weiner M, Segelmark M. The clinical presentation and therapy of diseases related to anti-neutrophil cytoplasmic antibodies (ANCA). Autoimmun Rev. 2016 Oct;15(10):978–982.
- Chirinos JA, Corrales-Medina VF, Garcia S, et al. Endocarditis associated with antineutrophil cytoplasmic antibodies: A case report and review of the literature. Clin Rheumatol. 2007 Apr;26(4):590–595.
- Li JS, Sexton DJ, Mick N, et al. Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis. 2000 Apr;30(4):633–638.
- Leavitt RY, Fauci AS, Bloch DA, et al. The American College of Rheumatology 1990 criteria for the classification of Wegener’s granulomatosis. Arthritis Rheum. 1990;33(8):1101–1107.
- Jennette JC, Falk RJ. Small-vessel vasculitis. N Engl J Med. 1997 Nov 20;337(21):1512–1523.
- Guillevin L, Pagnoux C, Seror R, et al. The Five-Factor Score revisited: Assessment of prognoses of systemic necrotizing vasculitides based on the French Vasculitis Study Group (FVSG) cohort. Medicine (Baltimore). 2011 Jan;90(1):19–27.
- McGeoch L, Carette S, Cuthbertson D, et al. Cardiac involvement in granulomatosis with polyangiitis. J Rheumatol. 2015 Jul;42(7):1209–1212.
- Walsh M, Flossmann O, Berden A, et al. Risk factors for relapse of antineutrophil cytoplasmic antibody-associated vasculitis. Arthritis Rheum. 2012 Feb;64(2):542–548.
- Lacoste C, Mansencal N, Ben M’rad M, et al. Valvular involvement in ANCA-associated systemic vasculitis: A case report and literature review. BMC Musculoskelet Disord. 2011 Feb 23;12:50.
- Anthony DD, Askari AD, Wolpaw T, McComsey G. Wegener granulomatosis simulating bacterial endocarditis. Arch Intern Med. 1999 Aug 9–23;159(15):1807–1810.
- Gerbracht DD, Savage RW, Scharff N. Reversible valvulitis in Wegener’s granulomatosis. Chest. 1987 Jul;92(1):182–183.
- Horino T, Takao T, Taniguchi Y, Terada Y. Non-infectious endocarditis in a patient with cANCA-associated small vessel vasculitis. Rheumatology (Oxford). 2009 May;48(5):592–594.
- Mishell JM. Cases from the Osler Medical Service at Johns Hopkins University: Cardiac valvular lesions in Wegener’s granulamatosis. Am J Med. 2002 Nov;113(7):607–609.
- Mortazavi M, Nasri H. Granulomatosis with polyangiitis (Wegener’s) presenting as the right ventricular masses: A case report and review of the literature. J Nephropathol. 2012 Apr;1(1):49–56.
- Ramakrishnan S, Narang R, Khilnani GC, et al. Wegener’s granulomatosis mimicking prosthetic valve endocarditis. Cardiology. 2004;102(1):35–36.
- Stollberger C, Finsterer J, Zlabinger GJ, et al. Antineutrophil cytoplasmic autoantibody-negative antiproteinase 3 syndrome presenting as vasculitis, endocarditis, polyneuropathy and Dupuytren’s contracture. J Heart Valve Dis. 2003 Jul;12(4):530–534.
- Varnier GC, Sebire N, Christov G, et al. Granulomatosis with polyangiitis mimicking infective endocarditis in an adolescent male. Clin Rheumatol. 2016 Sep;35(9):2369–2372.