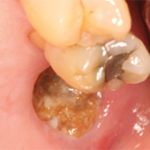
Medication-related osteonecrosis of the jaw (MRONJ) is a condition that manifests as exposed, necrotic and non-healing jaw bone in patients who have been treated with bisphosphonates, denosumab, chemotherapeutic agents, anti-angiogenic drugs, tyrosine kinase inhibitors, thalidomide and steroids.1-4 These medications are administered via intravenous, subcutaneous and oral routes to manage osteopenia; osteoporosis; hypercalcemia of malignancy; bone metastases of tumors including lung, prostate and breast; and the lytic lesions of multiple myeloma.4
Pathogenesis & Treatment
In patients with MRONJ, the mandible is twice as likely to be involved as the maxilla.4 Three theories have been proposed relating to the pathogenesis of MRONJ:4-6
- Inhibition of osteoclastic function and increase in osteoclast apoptosis, which negatively affect bone healing and remodeling;
- Inflammation and infection secondary to biofilms; and
- Interruption of vascular supply leading to osteonecrosis.
MRONJ’s four stages, stage 0 to stage 3, reflect disease severity.4 Based on the staging and severity of the condition, MRONJ can be managed surgically and/or non-surgically.4
The non-surgical therapeutic approach includes pain control, antibacterial mouth rinses, systemic antibiotics, pentoxifylline and alpha-tocopherol. Surgical treatment includes debridement and sequestrectomy, resection and reconstruction.7
Risk Factors
Dentoalveolar surgery increases the risk of MRONJ, with tooth extraction being the most common precipitating factor.4 In a study conducted by Saad et al., tooth extraction as a predisposing event was reported by 61% of patients with MRONJ.8 Similarly, Hoff et al. identified dental extraction as a risk factor in 55% of patients in their cohort who developed MRONJ.9
The above-mentioned studies included patients treated with intravenous and subcutaneous bisphosphonates.
Hasegawa et al., in their multicenter, retrospective study, documented the incidence of post-extraction MRONJ in patients who received oral bisphosphonates as 1.7%.10
The best current estimate for the risk of developing MRONJ in patients on oral bisphosphonates after tooth extraction is 0.5%, whereas the risk for patients with cancer exposed to intravenous bisphosphonates ranges from 1.6–14.8%.4
A study conducted by Yamazaki et al. on patients receiving oral bisphosphonates for more than three years has demonstrated delayed recovery, with persistent bone exposure in the extraction sockets at four weeks, suggesting delayed epithelialization may be a cause of MRONJ.11
Bisphosphonates & Delayed Wound Healing
Several researchers have investigated the complex relationship between bisphosphonates and oral tissue toxicity. The results of these studies have revealed decreased oral epithelial cell migration and apoptosis, further causing delayed oral mucosal wound healing.12
In 2008, Landesberg et al. studied the effects of pamidronate on oral mucosal cells in a murine model. They found oral epithelial proliferation and wound healing were inhibited at pamidronate concentrations above 0.1 mmol/L, thereby contributing to the development of MRONJ through persistent exposure of the underlying bone.13
Scheper et al. assessed the apoptotic effects of zoledronic acid on human gingival fibroblast and keratinocyte cell lines using an in vitro model. They concluded that the direct contact of clinically relevant concentrations of zoledronic acid causes apoptosis of epithelial and fibroblast cells.14
Cell death and suppression of epithelial proliferation ultimately leads to mucosal thinning and breakdown, causing bone exposure and rapid microbial colonization, resulting in MRONJ.5,14 Therefore, it can be concluded that epithelialization and mucosal healing is an essential step in the management of MRONJ.