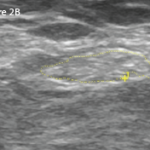
Sonography offers both qualitative and quantitative criteria to support the presence of CTS. Qualitatively, the median nerve may become hypoechoic and lose normal nerve echotexture.1 There may be swelling of the nerve proximal to the compression, and flattening of the nerve within a compression area. The abrupt flattening of the nerve is termed the “notch sign.”8
Various numeric sonographic criteria for CTS have been proposed, including direct measurement of CSA of the enlarged median nerve, comparison of CSA of the enlarged median nerve to the value in the forearm (i.e., the wrist-to-forearm ratio, or WFR), and the degree of palmar bowing of the flexor retinaculum.9-11
But how accurate is US in diagnosing CTS? A 2012 evidence-based guideline reviewed the four highest-quality studies up until May 2011 and determined the sensitivity of CTS diagnosis by US ranged from 65–97%, with accuracy ranging from 79–97%.5,12 These studies relied on median nerve CSA with the cut-off ranging from 8.5–10 mm2.
The conclusion: Based on Class I and Class II evidence, US measurement of median nerve CSA at the wrist is accurate and may be offered as a diagnostic test for CTS (Level A).12
What about Electrophysiological Studies?
Comparing US to EPS for CTS diagnosis may not be fair, because US delineates nerve structure and EPS looks at nerve function. In multiple studies, US and EPS featured fairly good correlation, although US correlated less well for mild CTS.13-16 We need further studies, though, before an abnormal US carries the same weight as an abnormal EPS in confirming CTS diagnosis.
What about patients with clinical CTS and negative EPS? As previously described, one study found completely normal EPS in 10–15% of cases of clinical CTS, and another study found 25% of CTS patients had normal EPS.6,17 A third study looked at 319 patients with a clinical diagnosis of CTS in whom 59 had normal EPS. US was performed on those 59 patients and compared with normal controls. US confirmed CTS in 18 of the EPS-negative 59 patients (i.e., about 30%).
The conclusion: US may be useful in diagnosing CTS in EPS-negative patients.18
How Do Orthopedists View US Diagnosis?
Not with any consensus. An evidence-based Level III meta-analysis of 19 articles (with a total of 3,131 wrists) published in an orthopedic journal in 2010 described US sensitivity and specificity of 77.6% and 86.8%, respectively. The authors suggested US, although not as sensitive or specific as EPS, may be a feasible alternative to EPS as a first-line confirmatory test.19 However, the February 2016 American Academy of Orthopaedic Surgeons’ CTS management guidelines support not routinely using US for the diagnosis of CTS due to limited evidence.20