These features included thick reticular dermal collagen bundles surrounded by clefts, adjacent dermal fibrocytes that stained with antibodies to CD34 and antibodies to procollagen I, and increased amounts of dermal mucin. (See Fig. 1) In deeper biopsies, Dr. LeBoit and colleagues occasionally observed angiogenesis within the septae of fatty lobules.2 They concluded that each patient had developed a novel skin disease that they named nephrogenic fibrosing dermopathy.3 Because fibrosis was subsequently observed in other organs, this entity has been renamed nephrogenic systemic fibrosis (NSF).
Faced with a potential emerging epidemic, the California Department of Public Health invited the Centers for Disease Control (CDC) to carry out an epidemiologic study of this novel skin disease. A case definition was established to identify patients who “developed large areas of hardened skin with slightly raised plaques, papules, or confluent papules with or without pigmentary alteration.” To confirm the clinical diagnosis, a skin biopsy demonstrating the novel characteristic histologic features was required.1
Unfortunately, the tragic events of September 11, 2001, forced the CDC to deploy its resources to other missions. By the time that Morbidity and Mortality Weekly Report featured “Fibrosing Skin Condition Among Patients with Renal Disease” as the lead article in its January 18, 2002, issue, 49 cases had been identified in the United States and Europe.1
When Endicott presented for dermatologic and rheumatologic evaluation at the academic medical center, she underwent a wedge biopsy of the skin on her leg that demonstrated characteristic changes of NSF. At the time of her evaluation, no treatment attempted previously had resulted in significant improvement of skin changes in patients with NSF. These treatments included potent topical and systemic corticosteroids, histamine H2-receptor antagonists, cyclosporine, intralesional interferon-a, psoralen with ultraviolet A light treatment, and plasmapheresis.4-6
Upon the recommendation of the dermatology consultant, Endicott was treated with thalidomide. However, thalidomide therapy did not bring about significant improvement of her skin thickening, tethering, or hyperpigmentation. She continued to experience progressively worsening pain and limited function. Endicott’s blood pressure began to drop precipitously during hemodialysis treatments. Eventually, she chose to terminate hemodialysis and she died 22 months after the onset of her skin changes. Since her death, decreased skin thickening and improved joint mobility have been reported in three patients treated with extracorporeal photopheresis, in three patients treated with plasmapheresis, in two patients treated with pentoxiphylline, and in one patient treated with high dose intravenous immunoglobulin.6-9
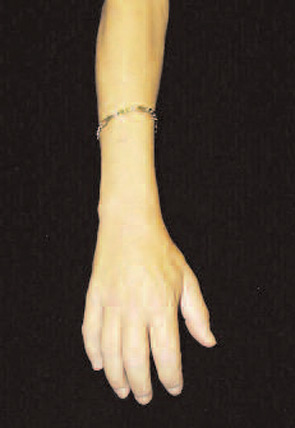
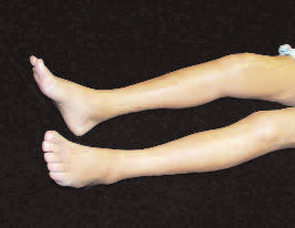
Investigation into NSF Causes
Although NSF most notably involves the skin, tissue obtained during surgery and at autopsy has revealed systemic involvement. Examination of striated and cardiac muscles has demonstrated muscle fiber atrophy, perimysial and endomysial fibrosis, calcium deposition, scattered interstitial chronic inflammation, and endomysial deposition of collagen fibrils.10 In the lungs, mild interstitial fibrosis, thickening of the adventitia of small- and medium-size arterioles, and fibrosis of the pleura and diaphragm have been observed.11,12 Cardiac involvement also occurs, with fibrosis of the pericardium, great vessels, left ventricle, and interventricular septum.13 Fibrotic changes of the genitourinary tract and of the dura mater also have been observed.
