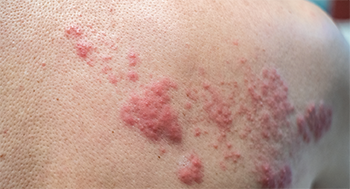
This rash shows the effects of varicella-zoster reactivation—shingles.
Mumemories / shutterstock.com
Varicella-zoster-virus (VZV) reactivation, which can cause patients to develop herpes zoster (i.e., shingles), occurs more frequently in patients with systemic vasculitis and systemic lupus erythematosus (SLE) who have received intravenous cyclophosphamide than in otherwise healthy adults, according to a retrospective study published in The Journal of Rheumatology by researchers in France.1 The study also shows that antiviral chemoprophylaxis with valacyclovir is an effective protective option for these patients.
“Zoster is an important burden for these patients, as described in our paper and papers from other groups. Moreover, when it occurs, it makes the choice of lowering the immunosuppressant treatment—or not—more difficult if the underlying disease is not under control,” says Guillaume Moulis, MD, PhD, assistant professor in internal medicine at the University of Toulouse, and one of the study’s co-authors.
Rheumatologists often prescribe intravenous cyclophosphamide to treat severe SLE flares and systemic vasculitis, along with corticosteroids. Cyclophosphamide exposure increases the risk of severe infections.2-4
Exploring Zoster Risks
The study’s goals were to assess zoster incidence and risk factors in patients with SLE or systemic vasculitis who have been exposed to intravenous cyclophosphamide.
Although evidence shows SLE patients are at higher risk for zoster, there had been little data on the risk among patients with systemic vasculitis.5 Past studies show that zoster is a concern for patients with granulomatosis with polyangiitis (GPA) and that treatment with corticosteroids and cyclophosphamide is a possible factor.6,7 In GPA, kidney failure may be one reason for this higher incidence of zoster.8
Because immunocompromised patients and those on moderate to high doses of immunosuppressive therapy, including cyclophosphamide, were excluded from clinical efficacy studies for the new recombinant zoster vaccine, Shingrix, the Centers for Disease Control and Prevention’s Advisory Committee on Immunization Practices (ACIP) does not currently recommend its use in these patients, although the committee will likely review these recommendations as more data become available.9 One of the aims of this study was to assess whether valacyclovir could be an effective, protective option for these patients.
“This study started from the experience of zoster flares in our patients, with a lack of data to explain the evolution of this to them, and from the observation that some patients had a chemoprophylaxis by valacyclovir, and others not,” says Dr. Moulis. “Consequently, we conducted this study to extend the knowledge about zoster in this setting, and to try to demonstrate the potential effectiveness of valacyclovir in this setting as well. These results impacted our practice.”
Since the study’s completion, physicians at his hospital now systematically prescribe valacyclovir for unvaccinated patients with the identified risk factors, says Dr. Moulis.