(click for larger image)
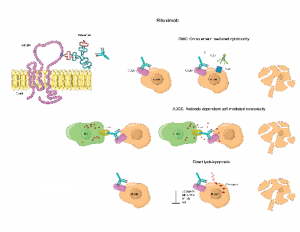
Rituximab is an antibody drug used to treat some cancers and autoimmune diseases.
ellepigrafica / SHUTTERSTOCK.COM
According to a large cohort study of pediatric patients, rituximab use is on the rise in the treatment of children diagnosed with vasculitis. Treatment with cyclophosphamide remains common, but it’s beginning to wane. Dialysis and mechanical ventilation also remain common, the study indicates.
The retrospective study of hospitalized children in the U.S. included the largest cohort of pediatric-onset anti-neutrophil cytoplasmic antibody (ANCA)-associated vasculitis (AAV) patients to date, according to lead author Karen E. James, MD, a pediatric rheumatologist who conducted the study while at Children’s Hospital of Philadelphia. The researchers published the study’s results, spanning more than a decade of data, in the September issue of Arthritis Care & Research.1
AAV causes inflammation of blood vessels that can lead to organ failure (mostly in the lungs and kidneys) and life-threatening morbidity. Dr. James says medical treatment for children with AAV is often based on physician experience combined with data learned from adult-only clinical trials.
“There has been a lot of research in the past 20 years looking at ANCA-associated vasculitis and its different subtypes in adults, and there have been a lot of advances in the medicines that treat them,” says Dr. James, now an instructor in pediatric rheumatology at the University of Utah School of Medicine and Primary Children’s Medical Center in Salt Lake City. “But nobody’s really looked at it in kids, and like a lot of rheumatologic diseases, it’s rarer in kids.”
The Rise of Rituximab

Dr. James
Historically, doctors have treated adults with high doses of glucocorticoids in combination with cyclophosphamide to induce remission. Cyclophosphamide is an immunosuppressive agent doctors also use in some forms of chemotherapy, and it’s been associated with serious morbidities, such as infection, hemorrhagic cystitis, infertility and malignancy, according to the study.
The treatment landscape began to change after two landmark studies in 2010 found that rituximab was not inferior to cyclophosphamide for the induction of remission of severe AAV, says Dr. James. Later studies showed the drug also proved efficacious in maintaining remission.2,3
“Our study demonstrates a gradual decline in the use of cyclophosphamide, a gradual increase in the use of plasma exchange and an exponential increase in the use of rituximab, indicating the data from the adult studies have influenced treatment paradigms in children,” the study authors write.