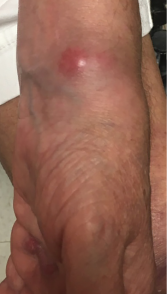
Figure 1. A lesion present on the patient’s left wrist at a clinic appointment in September 2018.
A 61-year-old white woman presented to our rheumatology clinic in New England to establish care in early June 2018, following a move from Texas. She reported a medical history of inflammatory bowel disease, uveitis and seronegative inflammatory arthritis, which was difficult to control and required the use of multiple medications.
At her initial visit, she reported taking 400 mg of hydroxychloroquine daily, 20 mg of methotrexate weekly, 5 mg of tofacitinib twice per day, 90 mg of ustekinumab weekly and 10 mg of prednisone daily. Ustekinumab was discontinued at that time due to a concern for excessive immunosuppression when used in combination with tofacitinib.
In early August 2018, she presented with new left wrist pain and swelling. Her exam was notable for diffuse metacarpophalangeal joint synovial thickening bilaterally and dorsal right wrist swelling with decreased flexion and extension due to pain. Her prednisone dose was briefly increased from 10 mg to 20 mg daily for the possibility that her wrist pain might represent an acute flare of inflammatory arthritis in the setting of discontinuation of ustekinumab.
In mid-August 2018, she underwent L5 decompressive lumbar laminectomy for central canal lumbar stenosis with radicular symptoms. Her course was complicated by postoperative fever. Urine showed greater than 100,000 cfu/mL Escherichia coli, for which she received a course of nitrofurantoin. By the end of August, she had fever recurrence. Computerized tomography (CT) scan of the lumbar spine showed a fluid collection concerning for abscess. Fluid aspirate was notable for pan sensitive Staphylococcus capitis, which grew only in broth media. She was started on six weeks of ceftriaxone and her remaining anti-rheumatic medications were discontinued; a prednisone taper was also initiated. Thereafter, she had no fever recurrence.
At her September 2018 rheumatology follow-up, she had profound swelling of her hands, especially the proximal interphalangeal joints, with wrist flexor and extensor tenosynovitis in both hands. Her left wrist showed a small, cystic-appearing lesion (see Figure 1). Her hydroxychloroquine was restarted and prednisone increased to 40 mg daily.
M. kansasii most typically causes pulmonary disease; however, it may also rarely manifest as skin & soft tissue, skeletal or disseminated disease.
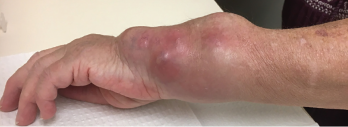
Figure 2. The patient’s left wrist at a clinic appointment in October 2018.
In October 2018, she returned to the rheumatology clinic acutely, due to rapidly progressive left wrist swelling and pain. The physical examination revealed a well-appearing patient with normal vital signs. The musculoskeletal exam was notable for marked swelling of the volar and ulnar aspects of the left wrist (see Figure 2).
Laboratory data revealed the values listed in Table 1 (see p. 60). Aspiration of the left wrist showed red, turbid fluid, 80,990 white blood cells/mcL (81% neutrophils) without crystals or organisms on Gram stain. Calcofluor white and acid-fast bacilli (AFB) stains were negative. A CT scan showed multiloculated fluid collections (see Figure 3) and associated bone destruction of the distal ulnar and radius (see Figures 4a and 4b), suspicious for osteomyelitis.
She underwent operative debridement of soft tissue and affected bone, with repeated specimen collection, with initial findings similar to the aspiration.
After six days, AFB culture grew an organism in liquid media; direct probe was negative for Mycobacterium tuberculosis and M. avium. In November 2018, the mycobacterial species was identified as M. kansasii, and she was started empirically on a daily, oral regimen of 1,000 mg of ethambutol, 300 mg of rifabutin and 250 mg of azithromycin.


