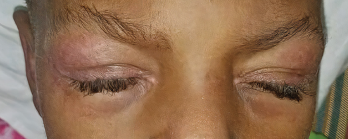
Photo 1: The patient presented with heliotrope rash.
Clinically amyopathic dermatomyositis (CADM), a rare subset of dermatomyositis (DM), is an autoimmune disease characterized by cutaneous findings of typical DM without evidence of myositis. Childhood presentation of CADM is rare, and not many studies describe the epidemiology of juvenile CADM.1,2
Although lung disease is rare among patients with juvenile DM, a few reports have been published since 2007 about interstitial lung disease (ILD) in children with CADM.3 Rapidly progressive ILD occurs more in CADM patients than in classic DM patients and has a poor prognosis.
Several studies have been conducted to find the association between specific autoantibodies and ILD in patients with CADM. Autoantibodies to a 140 kDa cytoplasmic protein (i.e., anti-CADM-140 antibodies) were first described in adults with CADM in Japan.4,5 The antibody is directed against an RNA helicase encoded by melanoma differentiation-associated gene 5 (MDA5), which is a pattern recognition receptor that can induce the transcription of type I interferon genes in response to viral infection.6
Later, a strong association was seen between rapidly progressive ILD and the presence of anti-CADM-140 antibodies, also known as anti-MDA5 antibodies, in juvenile patients with both classic DM and CADM.7 Patients with juvenile DM who have anti-MDA5 antibodies can develop rapidly progressive ILD, which is associated with a worse prognosis. Prompt and aggressive intervention may improve outcomes, but can sometimes be challenging due to difficulty recognizing the disease, in part because of heterogeneous presentations, and failure to respond to conventional immunosuppression.
We describe a 6-year-old patient who presented with Gottron papules, heliotrope rash, mild muscle weakness and persistent fevers.
Case Description
The patient is a 6-year-old Black child who presented with symptoms of mild muscle weakness and persistent fever up to 103ºF. The febrile episodes occurred almost every other day for about four to five months. He later developed joint pain, mainly involving his knees and elbows, with erythema and swelling. His mother noted a rash around her son’s eyes and on his hands about a month prior to presentation.
The patient was seen by his primary care physician and laboratory tests were obtained (see Table 1). The patient was referred to our hospital for further evaluation.
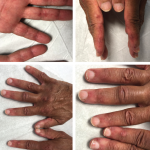
On examination, the patient was noted to have a heliotrope rash (see Photo 1) and Gottron papules (see Photo 2), Raynaud’s phenomenon and digital ulcers on the distal tips of his thumb, index and middle finger (see Photo 3); and mild weakness of his arms and legs.
Magnetic resonance imaging of both legs showed a mild increase in signal intensity in the rectus femoris, vastus lateralis, vastus intermedius and hamstring muscles in both legs. Treatment was initiated with 30 mg/kg/day intravenous steroids for three days and 10 mg of subcutaneous methotrexate once a week. He experienced an initial improvement of his weakness and rash. However, during the intervening four weeks before his follow-up appointment, the weakness and rash worsened. Steroid administrations were repeated, and 1 gm/kg intravenous immunoglobulin was administered once daily for two days.