Rheumatoid arthritis (RA) is a chronic, systemic, autoimmune disease with potential for multisystem involvement that promotes inflammation. Chronic inflammation of the synovial tissue results in stiffness, pain, warmth and swelling of joints. Untreated, it can lead to joint erosions and deformity resulting in disability and decreased quality of life (QOL). Both genetic and environmental factors have been implicated. Prevalence is estimated to be between 0.5 and 1.0% in the general population. Almost three times as many women as men have RA, with the highest incidence in middle age.1
Osteoarthritis (OA) is primarily the result of mechanical wear over time, leading to the loss of cartilage between the joints. It is the most common form of arthritis, affecting an estimated 12.1% of the U.S. population ages 25 and older. The prevalence of OA increases with age.2 Degenerative disk disease (DDD) is caused by daily stress on the spine and aging, which can be exacerbated by unnoticed major or minor injuries. Early changes of DDD can be apparent on radiographs in otherwise healthy adults between the ages of 30 and 50 years old, the majority of whom will be asymptomatic.3
Case Report
A 63-year-old woman with a 23-year history of RA presented with concern about her best treatment options. Due to multiple family relocations, she had seven previous rheumatologists. Her pharmacologic treatment over the years had included hydroxychloroquine, gold injections and, at one time, monotherapy with methotrexate (MTX). In 2002, infliximab was added to MTX, but efficacy waned, and she was switched to etanercept in 2008. Her major concern was fear of infection because she had recently experienced acute diverticulitis complicated by sepsis from a perforated bowel, requiring colostomy while she was taking combination therapy with MTX and etanercept. Both immunosuppressive agents were discontinued. After six-and-a-half months, she had a successful laparoscopic colostomy takedown.
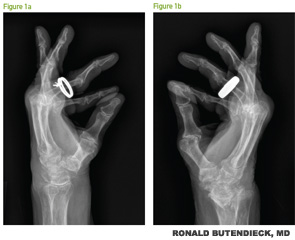
At the time of her visit, she was taking hydroxychloroquine 200 mg twice daily, as well as prednisone. Clinical evaluation demonstrated active bilateral polyarticular synovitis, flexion contractures and elevated inflammatory markers. Radiographs of the bilateral hands demonstrated changes consistent with severe, erosive, chronic rheumatoid arthritis (see Figures 1a and b, p. 50). Her prednisone was weaned off over the next six months, but secondary to persistent, active RA with elevated inflammatory markers, she agreed to start abatacept. At subsequent visits, progressive improvement was observed, and at six months, she achieved clinical remission.
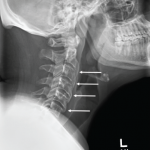
The patient also reported significant chronic neck pain with radicular symptoms that began after a fall in 1987. She was referred to a physiatrist and noted to have previously undetected DDD. Treatment included acetaminophen, nonsteroidal antiinflammatory drugs (NSAIDs), physical therapy, massage and relaxation training. Evaluation revealed diffuse weakness in her upper extremities, significant scapulothoracic dyskinesia with decreased range of motion and impingement of both shoulders, and reduction in lateral rotation of the cervical spine. She also had cervical facet discomfort. Reflexes were globally diminished. Radiographs of cervical spine noted DDD with multilevel facet arthrosis, but no subluxation at C1–C2 (see Figure 2, right). An MRI of the cervical spine did not demonstrate significant spinal stenosis or compressive lesions.
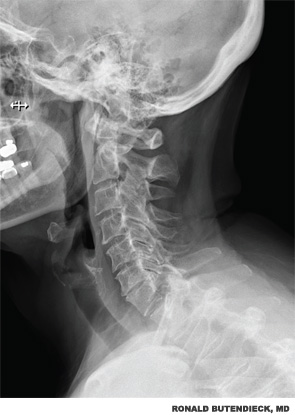
Electromyography did not demonstrate a cervical radiculopathy. Radiographs of the shoulders revealed acromioclavicular joint degenerative changes, marked glenohumeral joint space narrowing, and osteophyte formation with remodeling of the undersurface of the acromion bilaterally compatible with chronic rotator cuff arthropathy.
Fluoroscopically guided C7–T1 interlaminar epidural steroid injection was successful in alleviating her symptoms. The treatment plan combined physical therapy (PT) and occupational therapy (OT).
Discussion
RA and OA are both well-recognized clinical disease entities. This patient had both active erosive RA and untreated OA, contributing to her pain, decreased range of motion, weakness and reduction in QOL. She was assessed for both conditions, and a plan of care addressing each of these processes was put into action.
Conclusion
Multidisciplinary assessment and discussion among the rheumatologist, physiatrist, physical therapist, occupational therapist and the patient led to treatments for both RA and DDD, relieving years of unnecessary pain. Combination therapy with abatacept, hydroxychloroquine, acetaminophen, localized corticosteroid epidural injection, PT and OT enhanced her QOL.
In patients with RA, evaluation for other contributing causes for pain should be undertaken, especially for underlying OA. Early concomitant assessment and treatment of RA and OA may lead to better patient outcomes and QOL.
Patients who read and research information available to the general public from such sources as the ACR, Mayo Clinic brochures, Johns Hopkins brochures and white papers, and the Arthritis Foundation’s website can identify potential causes for their pain and enhance collaborative discussions with their clinical care physicians.
Patricia Frisch, PhD, LPC, LLC, is the corresponding author, an independent researcher, and retired director and owner of the Clinical and Pastoral Counseling Center and Allied Health Professional at Roper St. Francis Hospital in Charleston, S.C.
Ronald R. Butendieck, MD, is assistant professor of medicine in the Division of Rheumatology at the Mayo Clinic in Jacksonville, Fla.
Andy Abril, MD, is assistant professor of medicine in the Division of Rheumatology at the Mayo Clinic in Jacksonville, Fla.
Peter M. McIntosh, MD, is professor of physical medicine and rehabilitation in the Department of Pain Management at the Mayo Clinic in Jacksonville, Fla.
Salim M. Ghazi, MD, is assistant professor of anesthesiology in the Department of Pain Management at the Mayo Clinic in Jacksonville, Fla.
Elliot L. Dimberg, MD, is assistant professor of neurology in the Department of Neurology at the Mayo Clinic in Jacksonville, Fla.
Lynn F. Feldman, DO, is a physician in family medicine with Roper St. Francis Hospital in Charleston, S.C.
David G. Lucas, MD, is a general surgeon with Surgical Associates of Charleston, staff member at Roper St. Francis Hospital and Mount Pleasant Hospital in Charleston, S.C.
Andrea Styron, MRS-PT, is a physical therapist at Island Physical Therapy in Charleston, S.C.
References
- Ratini M., reviewer. Rheumatoid Arthritis Health Center: Slideshow: Understanding rheumatoid arthritis. WebMD. 2014 Apr 18. http://www.webmd.com/rheumatoid-arthritis/ss/slideshow-ra-overview.
- Nazario B, reviewer. Slideshow: A visual guide to understanding osteoarthritis. WebMD. 2014 Mar 4. http://www.webmd.com/osteoarthritis/ss/slideshow-osteoarthritis-overview.
- Nordquist C. What is degenerative disc disease? Medical News Today. 2014 Sep 26. http://www.medicalnewstoday.com/articles/266630.php#video-degenerative-disk-disease.