 ACR Convergence 2020—In the session titled Autoinflammatory Diseases: Mechanisms and Management, experts discussed the underlying immunopathology of autoinflammatory disease in adults.
ACR Convergence 2020—In the session titled Autoinflammatory Diseases: Mechanisms and Management, experts discussed the underlying immunopathology of autoinflammatory disease in adults.
Polly Ferguson, MD, a pediatric rheumatologist and director of the division of pediatric rheumatology at University of Iowa Stead Family Children’s Hospital in Iowa City, opened the session talking about SAPHO (i.e., synovitis, acne, pustulosis, hyperostosis and osteitis), a rare syndrome in adults characterized by skin and osteoarticular manifestations and one with many aliases, including CRMO (i.e., chronic recurrent multifocal osteomyelitis), a syndrome used in pediatric rheumatology and characterized by sterile osteomyelitis in one or more locations with or without skin, intestine or joint inflammation.
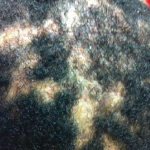
Both syndromes share similar clinical manifestations, including osteo-articular symptoms (e.g., pain, stiffness, joint swelling/warmth) and dermatologic symptoms (i.e., palmar-plantar pustulosis (PPP), psoriasis vulgaris and severe acne).
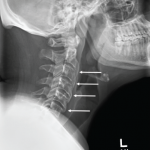
Although no validated diagnostic criteria currently exist for SAPHO, Dr. Ferguson pointed to criteria proposed by Kahn in 2003 in which osteitis/osteomyelitis is fundamental to the diagnosis.1 Specific inclusion criteria proposed by Kahn include bone-joint involvement with palmoplantar pustulosis, bone-joint involvement with severe acne, isolated sterile hyperostosis/osteitis and CRMO in children. Exclusion criteria include bone tumors and non-inflammatory condensing bone lesions, such as osteopoikilosis and steopathia striata.
Data from two studies describing the clinical features of SAPHO patients highlight the need for improved diagnosis, Dr. Ferguson said. A 1999 study of 120 patients by Haymen found 91% had osteitis and 84% had skin disease, with a median age of onset of 37.7 years and a delay in diagnosis of nearly 20 years after first clinical manifestations of disease.2 A more recent 2020 study of 249 patients with SAPHO with PPP or severe acne found a median age of disease onset of 20 years for those with severe acne and 37 years for those with PPP, with a seven-year delay in diagnosis for those with severe acne and a one-year delay for those with PPP.3
No validated diagnostic criteria currently exist for SAPHO.
Dr. Ferguson discussed the immunopathology of SAPHO in which immune dysregulation results in pro-inflammatory cytokine production, with genetic models supporting the role of interferon-1 (IL-1) in its pathogenesis.
Currently, SAPHO is treated empirically with off-label agents due to the lack of FDA-approved medications. Nonsteroidal anti-inflammatory drugs (NSAIDs) are used most often but are inadequate, she said, along with non-biologic disease-modifying anti-rheumatic drugs, including methotrexate, sulfasalazine and (more recently) Janus kinase inhibitors.