Increasingly, postmenopausal women are prescribed bisphosphonates in an effort to prevent osteoporotic fractures. The increased prevalence of bisphosphonate use likely reflects both demographic trends toward an older female population, as well as concerns about the safety of an alternative treatment for osteoporosis: hormone replacement therapy.
Increasingly, postmenopausal women are prescribed bisphosphonates in an effort to prevent osteoporotic fractures. The increased prevalence of bisphosphonate use likely reflects both demographic trends toward an older female population, as well as concerns about the safety of an alternative treatment for osteoporosis: hormone replacement therapy.
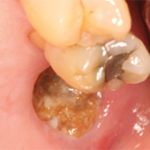
Unfortunately, bisphosphonates are not without risk. In 2008, the U.S. Food and Drug Administration (FDA) issued an alert that highlighted the association between oral bisphosphonates and incapacitating bone, joint and/or musculoskeletal pain. In 2015, the FDA issued yet another alert: warning that the use of bisphosphonates is associated with an increased risk for developing osteonecrosis of the jaw. Researchers have also noted that patients taking bisphosphonates experience an increased risk for arthritis and corresponding arthralgia. Now, investigators report that postmenopausal women who use bisphosphonates are also at increased risk for carpal tunnel syndrome.
Alfonso Carvajal, MD, a professor of pharmacology at the University of Valladolid in Spain, and colleagues published the results of their cohort study online on Jan. 14 in Plos One.1 The investigators designed their study in response to anecdotal reports of carpal tunnel syndrome in women prescribed oral bisphosphonates. They note in their paper that carpal tunnel syndrome is, unfortunately, associated with considerable employment and healthcare costs. Thus, the team designed its study to quantify the risk of carpal tunnel syndrome associated with bisphosphonate exposure.
The study used prospectively recorded information on the prescribing of oral bisphosphonates from The Health Improvement Network (THIN) database. The large database includes the primary healthcare records of patients throughout the U.K. To be included in the study, patients had to be registered in the database for more than one year. The investigators determined exposure based on the prescription of an oral bisphosphonate. They did not collect self-reported drug use. The large study included 59,475 women of more than 51 years old who received at least one prescription for oral bisphosphonates. The study included up to 11 years of data on these individuals.
The investigators found 19,825 women were prescribed bisphosphonates during the study period. This translated into an exposed cohort of 51,245 person-years of follow-up. They then compared those women who were prescribed bisphosphonates with those who were not. They found no difference in age distribution or mean follow-up between the two groups.
The researchers identified which women had carpal tunnel syndrome as documented in their medical records. Of the 572 total women diagnosed with carpal tunnel syndrome, 242 were exposed to bisphosphonates and 330 were unexposed. The investigators calculated that women exposed to bisphosphonates had an adjusted hazard ratio of 1.38 (95% confidence interval, 1.15–1.64) for developing carpal tunnel syndrome when compared with women who were unexposed. However, when they analyzed different levels of bisphosphonate exposure, they were unable to identify a relationship between level of exposure and increasing risk.