
Cocaine-related vasculopathy presents a unique diagnostic challenge. It resembles systemic vasculitis in clinical and laboratory findings but lacks confirmatory evidence of vasculitis on biopsy. The stigma associated with drug use often makes it difficult to obtain an accurate history. In this report, we describe four female patients with cocaine-related skin necrosis. The clinical and serological profiles in these cases led to the initial differential diagnosis of antiphospholipid syndrome, cutaneous vasculitis, cryoglobinemia, or systemic lupus erythematosus (SLE). However, skin biopsies revealed mainly microvascular thrombosis with only minimal evidence of leukocytoclastic vasculitis. These atypical histological findings, combined with a positive urine toxicology screen for cocaine, suggest vasculopathy induced by levamisole, an adulterant used as a cutting agent in cocaine.
The Cases: Patient 1
A 49-year-old black female presented to the outpatient rheumatology clinic with a five-month history of intermittent bilateral knee swelling and pain. She also noted fatigue, myalgias, painful oral ulcers, and a 20-pound weight loss. Right knee arthrocentesis revealed nucleated cells (9,720), no crystals, and negative cultures. Serological testing was significant for positive antinuclear antibody (ANA) 1:320 with a speckled pattern, an anti–double stranded DNA (anti-dsDNA) of 235.5 IU/ml (normal < 30) negative rheumatoid factor (RF), anticitrullinated cyclic peptide (anti-CCP), cryoglobulins, and normal complement levels. A lupus anticoagulant (LAC) screen was positive, but a dilute Russell viper venom time (dRVVT) confirmatory test was negative. The anti–beta-2-glycoprotein and anticardiolipin (ACL) antibodies were both negative. Inflammatory markers were notable for an elevated erythrocyte sedimentation rate (ESR) of 63 mm/hr and C-reactive protein (CRP) of 138 U. Based on her clinical presentation and positive serologies, the patient was diagnosed with SLE. Her right knee was injected with corticosteroids, and she was started on hydroxychloroquine (HCQ) 400 mg/day.
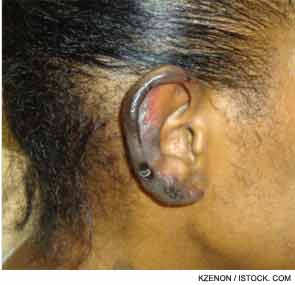
She returned two weeks later with a new purpuric necrotic rash on both external ears and on the upper and lower extremities, accompanied by intense pain (see Figure 1). She denied any cold exposure or Raynaud’s phenomenon, but was noted to have oral and nasal ulcers. Upon further questioning, the patient admitted to using inhaled cocaine prior to the development of her skin lesions. A urine drug screen for cocaine was positive. Additional serologic testing revealed a positive antineutrophilic cytoplasmic antibody (ANCA) of 1:320 initially and 1:640 on repeat testing. Myeloperoxidase (MPO) was 34 U (normal=negative 0–20 units, weakly positive 21–30 units, moderate to strongly positive >30 units), and anti–proteinase-3 (PR3) was 47 (normal=negative 0–20 units, weakly positive 21–30 units, moderate to strongly positive >31 units). Skin biopsy findings are shown in Figure 2 and summarized in Table 1. A presumptive diagnosis of cocaine/levamisole-associated vasculitis was made. The patient was counseled to abstain from further illicit drug use.
