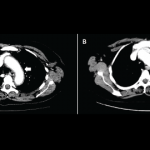
Any immune system-mediated tissue damage secondary to ICIs is known as an irAE. irAEs vary in severity and can involve any organ system, but most commonly affect the skin, gastrointestinal tract, endocrine glands such as the thyroid and pituitary, and less commonly the lungs (see Figure 2).9 Rare adverse events are being increasingly recognized, as in a recently published report of two patients who developed fatal myocarditis after treatment with ipilimumab and nivolumab.10
Development of irAEs typically occurs within several weeks of beginning immunotherapy. As noted in clinical trials, the majority of high-grade irAEs related to PD-1 inhibitors occur during the first 12–14 weeks of treatment.11 Combination therapy with nivolumab plus ipilimumab may result in irAE development earlier and more frequently than with monotherapy. This has ranged from skin manifestations at two weeks, GI symptoms at seven weeks, and hepatic and endocrine dysfunction between nine and 12 weeks.12,13
irAEs from ICIs are increasingly recognized as unique entities mimicking traditional rheumatic diseases.14 In a case series of 13 patients treated with nivolumab and/or ipilimumab, nine developed an inflammatory arthritis, and four developed sicca syndrome. The arthritis patients reported in this series were negative for rheumatoid factor and anti-cyclic citrullinated peptide antibodies. In the case of sicca syndrome, dry mouth tended to be more severe than dry eyes.15 Biopsy-proved giant cell arteritis and lupus nephritis have also been reported.16,17 Inflammatory muscle disease has been noted rarely with descriptions of both polymyositis causing significant respiratory muscle weakness and classic dermatomyositis with V-sign and heliotrope rash.
A severe case of dermatomyositis related to ipilimumab therapy for metastatic melanoma has been reported with initial resolution of signs/symptoms on steroids and discontinuation of ICI therapy.18 Interestingly, when the patient’s cancer recurred, she was again treated with ipilimumab, with prompt return of dermatomyositis.
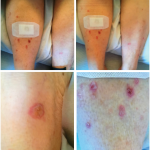
Dermatologic irAEs may be mild to severe. According to a recent meta-analysis, development of a rash with ipilimumab is fairly common, with mild cases occurring in about 24% of patients and high-grade rashes occurring in only 2%.19 The rashes are typically erythematous macules and papules and were not found to be dose dependent. Vitiligo and pruritus have also been seen with use of ipilimumab.
Gastrointestinal irAEs include colitis, diarrhea, obstruction, perforation and toxic megacolon.11 Diarrhea is most pronounced in combination therapy. Similarly, hepatotoxicity is common and when it is severe, can result in AST, ALT and bilirubin levels greater than 20 times the upper limit of normal, with fulminant hepatic failure.